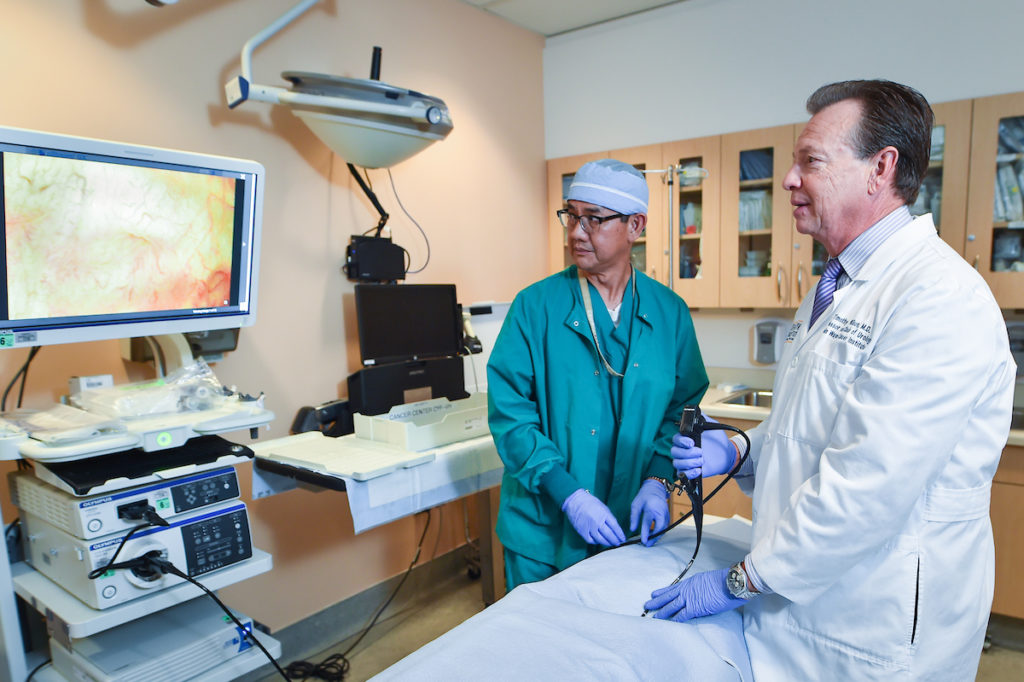
Written by Timothy Wilson, M.D., Professor and Chair of Urology and Urologic Oncology at the Saint John’s Cancer Institute.
Years of controversy and uncertainty of whether regular screening for prostate cancer is beneficial, have led many men to stop getting screened all together. According to the American Cancer Society, they recommend that men make an informed decision with their physician about the screening, in order to better understand the risks and benefits.
Timothy Wilson, M.D., professor and chair of urology, said he has seen an increase in aggressive prostate cancer because of late screenings. This is partly due to men not completely understanding both sides of this screening debate.
Below, Dr. Wilson provides his assessment on prostate cancer screening based on his own experience.
What is a prostate cancer screening?
The prostate-specific antigen (PSA) blood test is one of the first tests done in men who have symptoms of prostate cancer. Men with a PSA level between 4 and 10 have about a 1 in 4 chance of having prostate cancer. If the PSA is above 10, the chance of having prostate cancer is more than 50 percent. Sometimes this screening is done in conjunction with a digital rectal exam.
Although the PSA test is not perfect, it is very reliable in finding early prostate cancer. Historically, since 1990, when prostate cancer screening originated, death rates have fallen by 30 percent. With screening, you can decrease the number of men that die from prostate cancer. Screenings performed on a regular basis can find cancer in its earliest stages, resulting in having the best possible chance of curing it.
What are the screening guidelines that you recommend?
Men that need to be screened are men who are at risk for prostate cancer, which includes:
- All men above the age of 50, because incidence begins to rise around that age. Prostate cancer is rare in men younger than 40, unless they have certain risk factors like;
- African American men, who have an increase risk in prostate cancer, and;
- Men who have first degree relatives with prostate cancer, so brothers or fathers.
- Men with diets high in red meat and low in fruits and vegetables have a higher risk of prostate cancer.
What are the potential harms and benefits? Why is there controversy surrounding this screening?
Because prostate cancer is a slow growing cancer, the criticism with screening for it, is that physicians are going to over-diagnose cancers that don’t need to be treated. Also, fear and anxiety can take a toll a However, what is important is to diagnose cancer as early as possible, so we can find it when it is still confined to the prostate and has not yet spread.
Prostate cancer is a common disease, so it makes sense to screen for it, unlike, testicular cancer, for example, which is rarer, so mass screenings are not the best option. Yes, the biopsy is invasive and is done under local anesthesia in the doctor’s office, while men are awake. It only takes about 10 minutes, but it is uncomfortable and somewhat painful, and there are some risks, like bleeding and the potential for serious infections. However, serious bleeding and infections are rare.
So, for men who have an abnormal PSA, the likelihood of finding prostate cancer is about 30 to 50 percent, and on the flip side about 70 percent of men will have had an unnecessary biopsy. However, a PSA by itself is still the best screening mechanism.
What advice would you share with someone facing a medical decision?
I like to tell my patients that it is best to work from a foundation of knowledge, as appose to ignorance. It is better to know what you are dealing with. Understanding and learning about your diagnosis and options, helps you make a more informed decision when planning, not only your treatment plan, but how it all affects your day to day life.
Also, there isn’t one treatment that fits all men. Tailoring the treatment to each individual and each circumstance is in the details of a person’s cancer, it is what needs to be done.
Learn more about our urologic oncology services at the Saint John’s Cancer Institute. To make an appointment, please call (310) 582-7137.

