March is Kidney Cancer Awareness Month.
So, why is that important?
Unlike many other types of cancers that may affect us in our lifetime, kidney cancer can be challenging to detect. Without a clear set of symptoms, which could be mistaken for other problems, there is no screening mechanism for kidney cancer. While there are known risk factors that increase with age, including tobacco use, obesity, other health problems, as well as environmental factors, most kidney cancers are found by chance.
The most common type of kidney cancer is Renal Cell Carcinoma (RCC), referred to as, clear cell. The impact on the U.S. population reveals a 2 percent risk for men and a 1 percent risk for women1, which is consistent with kidney cancer occurrence, where about 65 percent of cases affect men and about 35 percent affect women. Kidney cancer is often found through unrelated medical exams. A CT scan, for example, may indicate a visible tumor on or inside the kidney, which would be cause for additional evaluation and treatment. There are physical symptoms that could be a sign of kidney cancer that can manifest separately or together, including rust or pink-colored blood in the urine, pain in the side and black that doesn’t go away, unexplained weight loss, and feeling very tired.
If smaller kidney tumors are easier to treat, how do you find them?
Though kidney cancer is difficult to detect, the good news is that there is a link between the tumor size and the likelihood that it has not spread to other parts of the body (metastasis). A small mass suggests a localized or benign tumor—one that has not spread. This dynamic may help with staging and determine how soon treatment is needed. Kidney cancer can often be cured if diagnosed and treated when it is still localized to the kidney.
For kidney cancer, the most important thing is the size of the tumor that’s in the kidney. The bigger the tumor, the higher the risk that you might have cancer [spread] outside the kidney.
– Jennifer Linehan, MD
Like other detectable cancers, the hope is to reach a definitive diagnosis through something as simple as a blood or urine test, creating the starting point of what could lead to new healthcare recommendations. Achieving this goal would give you and your doctor information on what to look for and when to screen.
Dr. Jennifer Linehan explains incidental kidney tumors.
Dr. Linehan discusses why symptoms of kidney cancer are rare and difficult to detect, and how we continue to make progress to identify kidney cancer using biomarkers.
How do you treat Non-clear Renal Cell Carcinoma (RCC)?
There are many subtypes of renal cell carcinoma called non-clear cell RCCs that respond differently to treatment, so it varies. The challenge in the research is to find the best treatment approach for each of these subtypes. While they do not respond as well to targeted therapy drugs as other cancers do and can have poorer outcomes1, combining these treatments is making a difference.
Do I have to remove my kidney?
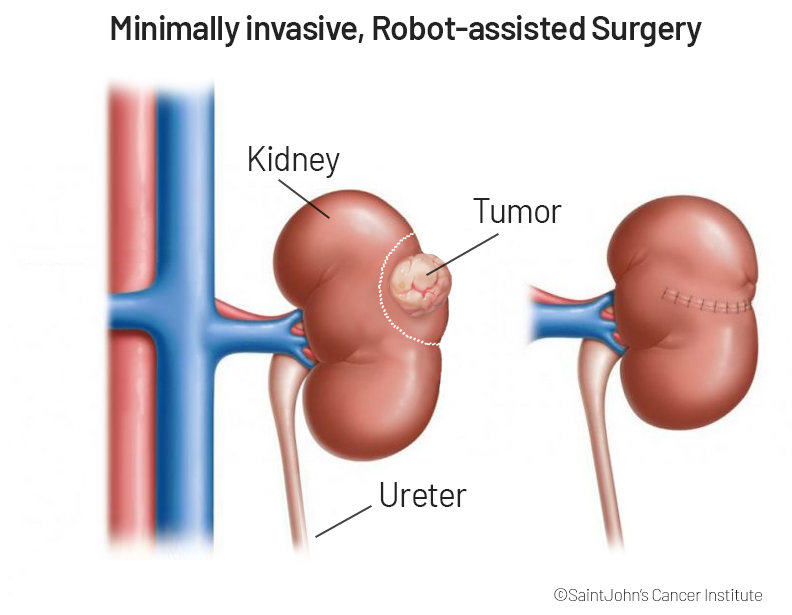
Not necessarily… Through minimally invasive robotic surgery, we can limit surgery to just the area around the tumor, sparing most of the kidney and avoiding the need for complete kidney removal (nephrectomy). See Kidney Cancer: Symptoms, Risk Factors, Diagnosis, Stages, and Treatment. This minimally invasive approach aims to preserve kidney function, which is better for the patient and their recovery.
Surgery is the primary treatment for most kidney tumors. Among other treatments, radiation may be used to treat kidney cancer if the patient has only one kidney or is not healthy enough to have surgery.1
…I do complex reconstruction of the kidney, so if the mass is small enough, you might not want to remove the whole kidney and just the mass itself. But if the mass is close to the vessels of the kidney, we might have to reconstruct or repair those vessels so that we can preserve most of the kidney.
– Jennifer Linehan, MD
What about Targeted therapy and Immunotherapy?
Studies have recently indicated who benefits most from targeted therapy and immunotherapy. When targeted and immunotherapy are used in combination, they can provide the first line of defense for kidney cancers that have spread beyond the kidney or that cannot be removed by surgery. Sometimes targeted therapy is given before surgery to shrink the tumor (neoadjuvant therapy), which can reduce the extent of surgery needed and preserve kidney function. Receiving targeted drugs after surgery (adjuvant therapy) is also being researched to validate they can reduce the chances of cancer recurrence.1 Chemotherapy is not effective against kidney cancer.
Kidney Cancer Treatment Options:
- Surgery (a robotic/minimally invasive procedure to remove the tumor or kidney)
- Targeted Therapy and Immunotherapy (involves drugs that can be used together to shrink the tumor
- Radiation Therapy (uses concentrated X-rays to shrink and kill tumor cells)
- Cryotherapy (freezes and kills tumor cells)
- Microwave Ablation (destroys tumor cells using heat)
What is Radiation Therapy for Kidney Cancer?
Radiation therapy for kidney cancer, also known as renal cancer, is less standard than other treatments but is used in specific cases. This therapy involves using high-energy rays to target and kill cancer cells. It is typically considered when surgery is not an option or for palliative care to relieve symptoms like pain.
What is Cryotherapy?
Cryotherapy, a standard treatment for kidney cancer, involves freezing renal tumors to destroy cancer cells. This minimally invasive procedure uses a probe inserted through the skin into the cancer, guided by imaging techniques. Cryotherapy is suitable for small tumors or patients who cannot undergo surgery and offers a compelling alternative, especially for early-stage kidney cancer.
What is Microwave Ablation?
Microwave ablation, a standard treatment for kidney cancer, uses heat generated by microwave energy to destroy renal tumors. This minimally invasive procedure involves inserting a thin probe into the tumor, guided by imaging techniques. It is most effective for small tumors or patients who cannot undergo surgery.
Known and newly established risks
Since the turn of the century, we have understood how excessive meat consumption is linked to increased cancer risk. Studies published by the Center for Disease Control (CDC) reveal a positive relationship between meat consumption and the risk of renal cell carcinoma, indicating a “20% to 22% higher risk of renal cancer” while eating red meat; in addition, was associated with 27% and 30% higher risk.” This finding, which included red meat and processed meat, was associated with an increased risk of kidney cancer.2 Reducing meat consumption is a meaningful approach to decreasing the rate of kidney cancer.
What about risks due to chemical exposure?
Avoid hazardous chemicals at all costs, especially if exposure is extended over a long period. In a large, comparative, occupational study of autoworkers who were regularly exposed to metalworking fluids (MWF)—synthetic and soluble liquids used to cool and lubricate metals—a relation was found between cumulative exposure and a linear increase in renal cell carcinoma.3 In addition, an “increased risk” of renal cell carcinoma has been linked to individuals with high exposure to Perfluorooctanoic Acid (PFOA), which can be found in chemical plants, work environments, or homes with contaminated drinking water. PFOAs are found in a variety of common products such as cookware, paper food packaging, carpet, personal care items, and other commodities. PFOAs are a “suspected endocrine (hormone) disruptor” that is also linked to fertility problems.4 These chemicals and others that are known for their carcinogenetic properties are found in many industries. Limiting your exposure to these chemicals is the only way to avoid such risk.
Common Questions about Kidney Cancer
Does kidney cancer spread quickly?
Kidney cancer, also known as renal cancer, varies in how quickly it spreads depending on its type and stage at diagnosis. Renal cell carcinoma, the most common type, typically grows slowly. However, some subtypes, like sarcomatoid renal cell carcinoma, can be more aggressive.
- Growth Rate: Varies by cancer type and stage.
- Common Type: Renal cell carcinoma usually grows slowly.
- Aggressive Forms: Certain subtypes may spread quickly.
Transitioning to advanced stages, the cancer can spread to other organs, including the lungs and bones.
How is kidney cancer usually found?
Kidney cancer is usually found incidentally during imaging tests for unrelated conditions. Common methods include ultrasounds, CT scans, and MRIs, which can detect tumors in the renal area. Symptoms like blood in the urine, back pain, or unexplained weight loss might also prompt further investigation.
What is the life expectancy of someone with kidney cancer?
The life expectancy of someone with kidney cancer varies based on the stage at diagnosis and the effectiveness of treatment.
- Localized Cancer: Five-year survival rate1 of 93%.
- Regional Spread: Five-year survival rate1 of 70%.
- Distant Metastasis: Five-year survival rate1 of 12%.
What is the typical age for kidney cancer?
Kidney cancer, also known as renal cancer, is most commonly diagnosed in people aged 60 to 702, with the average age at diagnosis being around 65. Although it can occur at any age, it is rare in individuals under 45.
References:
- Survival rates for kidney cancer. American Cancer Society. (n.d.). https://www.cancer.org/cancer/types/kidney-cancer/detection-diagnosis-staging/survival-rates.html
- Fast facts. Kidney Cancer Association. (2024, March 25). https://www.kidneycancer.org/fast-facts/
Learn more about Kidney Cancer and Surgical Treatment
- Surgery for Urologic Cancers
- Kidney Cancer: Symptoms, Risk Factors, Diagnosis, Stages, and Treatment
- Get answers to your questions: Request an appointment with Dr. Linehan.
Sources
1 Cancer.org. (2023). Key Statistics About Kidney Cancer.https://www.cancer.org/cancer/kidney-cancer/about/key-statistics.html
2 CDC.gov. (2007). Faramawi, M.F., Johnson, E. Fry, M.W. et al. Consumption of different types of meat and the risk of renal cancer: meta-analysis of case–control studies. Cancer Causes Control. https://doi.org/10.1007/s10552-006-0104-9
3pubmed.ncbi.nlm.nih.gov. (2016). Deepika Shrestha, Sa Liu, S. Katharine Hammond, et al. Risk of renal cell carcinoma following exposure to metalworking fluids among autoworkers. Occup Environ Med. https://pubmed.ncbi.nlm.nih.gov/27484955/
4National Cancer Institute. (2017). DCEG Staff. Environmental Pollutant, PFOA, Associated with Increased Risk of Kidney Cancer. https://dceg.cancer.gov/research/what-we-study/pfas