What is Liver Cancer?
Liver cancer is a disease of the liver that can develop as a primary or a secondary cancer (spread from another organ). It can be caused by several conditions including hepatitis B virus (HBV), hepatitis C virus (HCV), chronic long-term infection, fatty liver disease, primary biliary cirrhosis (PBC), excessive alcohol consumption, and various chemicals such as aflatoxins known to damage the DNA in liver cells.
Studies have shown that aflatoxins can damage the TP53 tumor suppressor gene, which normally works to prevent excessive cell growth and division. Damage to the TP53 gene can lead to increased growth of abnormal cells and formation of cancer in the liver. Infection of liver cells with hepatitis viruses can also damage DNA. These viruses have their own genetic profile that carries instructions on how to infect cells and produce more viruses. In some patients, this viral DNA can insert itself into a liver cell’s DNA where it may affect the cell’s genes, which can develop into cancer. The most significant risk factor for liver cancer is chronic infection from contracting hepatitis B and C viruses. These viruses can spread from person to person and therefore can be prevented by avoiding activities that transfer fluids of the body.
Types of Liver Cancer
Tumors are abnormal masses of tissue that form when cells begin to reproduce uncontrollably. Both noncancerous (benign) and cancerous (malignant) tumors can develop in the liver.
Noncancerous liver tumors
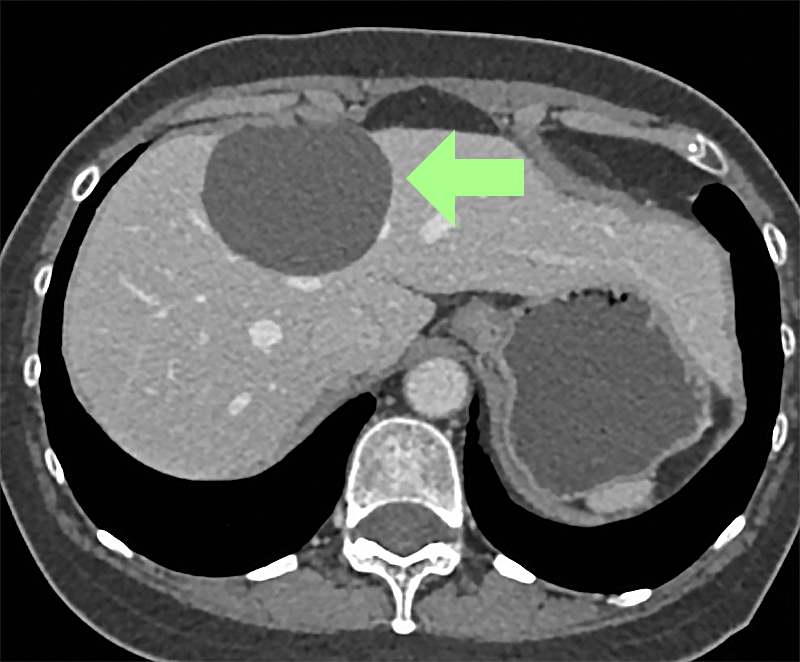
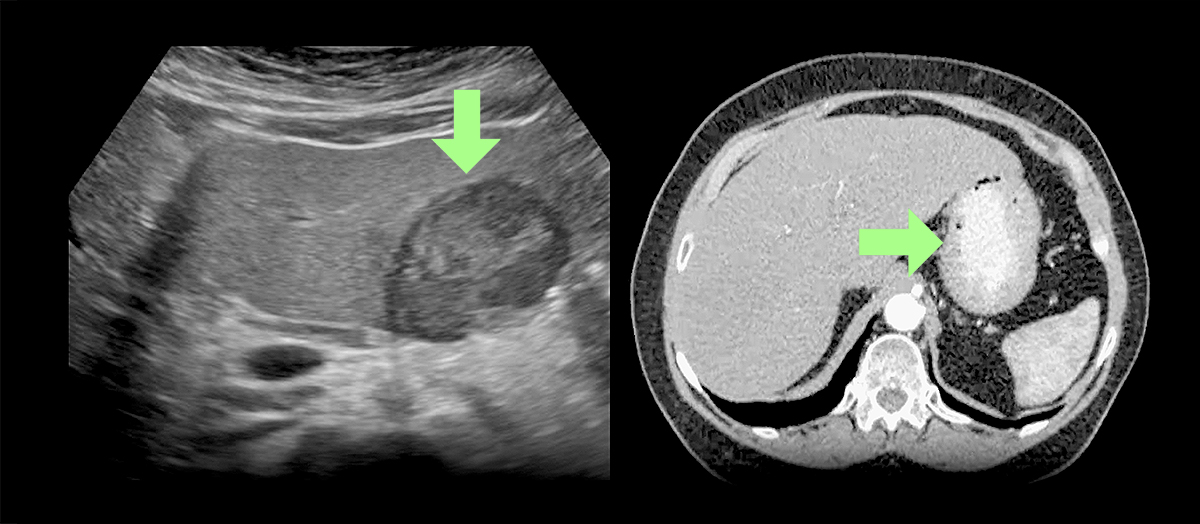
Noncancerous tumors are common and usually have no symptoms. In fact, if they’re found at all, it’s because the patient has undergone an ultrasound, CT, or MRI scan, revealing the location of the tumor among the health tissues or organ. Generally, benign tumors are not a serious health condition. However, benign tumors can sometimes grow large enough to cause serious problems, which may require medical intervention or preventive treatment. Unlike cancerous growths, benign tumors do not spread to nearby tissues, the lymphatic system, or to distant parts of the body. If they need to be treated, they can be removed successfully with surgery.
Hemangioma
The most common type of benign liver tumors is called hemangiomas, which start in blood vessels. Most hemangiomas of the liver cause no symptoms and do not need treatment. However, some may bleed or become large enough to cause pain and may need to be removed surgically.
Hepatic adenoma
Hepatic adenoma is a benign tumor that starts from the main type of liver cell called hepatocytes. Most do not cause symptoms and do not need treatment. Some eventually do cause problems, such as pain or a mass in the stomach, or blood loss. Because there is a risk that the tumor could rupture, leading to severe blood loss as well as a small risk that it might eventually develop into liver cancer, we may recommend surgery to remove the tumor.
Focal nodular hyperplasia
Focal Nodular Hyperplasia (FNH) is a tumor-like growth made up of several cell types (hepatocytes, bile duct cells, and connective tissue cells). Although FNH tumors are benign, it can be hard to tell them apart from true liver cancers, and we often remove them surgically when the diagnosis is unclear.
Liver cysts
An estimated five percent of the population develop liver cysts. They are benign growths that contain fluid produced by the cell wall of the cyst. Most cysts do not need therapy, but some can grow and be large enough to cause pain. These can be drained laparoscopically as an outpatient procedure to alleviate symptoms.
Cancerous liver tumors
Cancerous or malignant liver tumors can either originate in the liver (known as primary liver cancer) or spread to the liver from another cancer elsewhere in the body (metastatic liver cancer). Most cancerous tumors in the liver are metastatic.
Hepatocellular carcinoma:
Also known as hepatocellular cancer, or HCC, this is the most common form of liver cancer in adults. It is also sometimes called hepatoma. About 4 of 5 cancers that start in the liver are this type.
Hepatocellular cancer can have different growth patterns:
- A single tumor that grows larger. Only late in the disease does it spread to other parts of the liver.
- Small cancer nodules throughout the liver, not just a single site. This is seen most often in people with cirrhosis (chronic liver damage).
Chronic infection with hepatitis B and C increases the risk of developing this type of cancer. In addition to cirrhosis, other causes include certain chemicals and alcoholism.
Under a microscope, we can distinguish several subtypes of HCC. Most often these subtypes do not affect treatment or the prognosis for survival. However, one of these subtypes, fibrolamellar, is important to recognize. This type is rare, does not affect the entire liver, and make up less than one percent of HCCs diagnosed. Patients with this type are usually younger than age 35 while there is generally a better outlook for this subtype than other forms of HCC.
Bile duct cancer (Intrahepatic cholangiocarcinoma):
The bile duct starts in the liver. Smaller tubes that are like small blood vessels drain bile from the cells in the liver into larger and larger branches, ending in a tube referred to as the common bile duct. Bile duct cancer begins when normal cells in the bile duct change and grow uncontrollably forming a mass called a tumor, which can be benign or malignant. About 10 to 20 percent of liver cancers are bile duct cancers. Surgical removal of these tumors offers the best chance for cure.
Angiosarcoma and hemangiosarcoma
Angiosarcoma and hemangiosarcoma are both rare cancers that begin in cells lining the blood vessels of the liver. People who have been exposed to vinyl chloride or to thorium dioxide are more likely to develop these cancers. It’s also possible that exposure to arsenic or radium could lead to this type of liver cancer. There is also an inherited condition known as hemochromatosis that can also lead to these types of tumors.
Angiosarcomas and hemangiosarcomas can grow quickly. By the time they’re found, these tumors are often too widespread to be removed surgically. Chemotherapy and radiation therapy may help slow the spread of the disease, but these cancers are usually very hard to treat.
Hepatoblastoma
This is a very rare kind of cancer that develops in children, usually in those younger than four years old. The cells of hepatoblastoma are similar to fetal liver cells. About two out of three children with these tumors are treated successfully with surgery and chemotherapy, although the tumors are harder to treat if the cancer has spread outside of the liver.
Secondary or metastatic liver cancer
Most of the time when cancer is found in the liver, it did not start there. Instead, it spread or metastasized from somewhere else in the body, such as the pancreas, colon, stomach, breast, or the lung. These tumors are named and treated based on where they originated. For example, if your cancer started in the lung and spread to the liver it’s still called lung cancer with spread to the liver, not liver cancer, and it is treated as lung cancer. Treating the cancer according to its origin provides the most optimal treatment with increased success.
Symptoms of Liver Cancer
Many patients with primary liver cancer have no symptoms. However, the following are the most common symptoms of a developing liver tumor or hepatoma:

- Abdominal pain
- Loss of appetite
- Fatigue
- Bloating
- Weight loss
- Nausea
- Vomiting
- Large mass that can be felt in upper-right part of the abdomen
- Fever
- Jaundice or yellowing of the skin and eyes, and a darkening of the urine
- Persistent itching
- Swelling of the legs
- A general feeling of poor health and weakness
The symptoms of a liver hepatoma may resemble other medical conditions or problems. Always consult your surgeon for a diagnosis.
The following are the most common symptoms of metastatic liver cancer:
- Weight loss
- Poor appetite
- Enlarged, hard, and tender liver
- Fever
- Enlarged spleen
- Ascites or fluid buildup in the abdominal cavity
- Jaundice or yellowing of the skin and eyes
- Confusion
- Drowsiness
The symptoms of metastatic liver cancer may resemble other medical conditions or problems. Always consult your doctor for a diagnosis.
Diagnosing Liver Cancer
Diagnosing liver cancer or metastatic liver cancer may include one more tests. They include blood tests and imaging tests, such as a CT scan, ultrasound, and MRI. It is sometimes necessary to remove a sample of liver tissue for biopsy.
Testing methods
One or more tests may be needed to determine the extent of cancer spread and its stage.
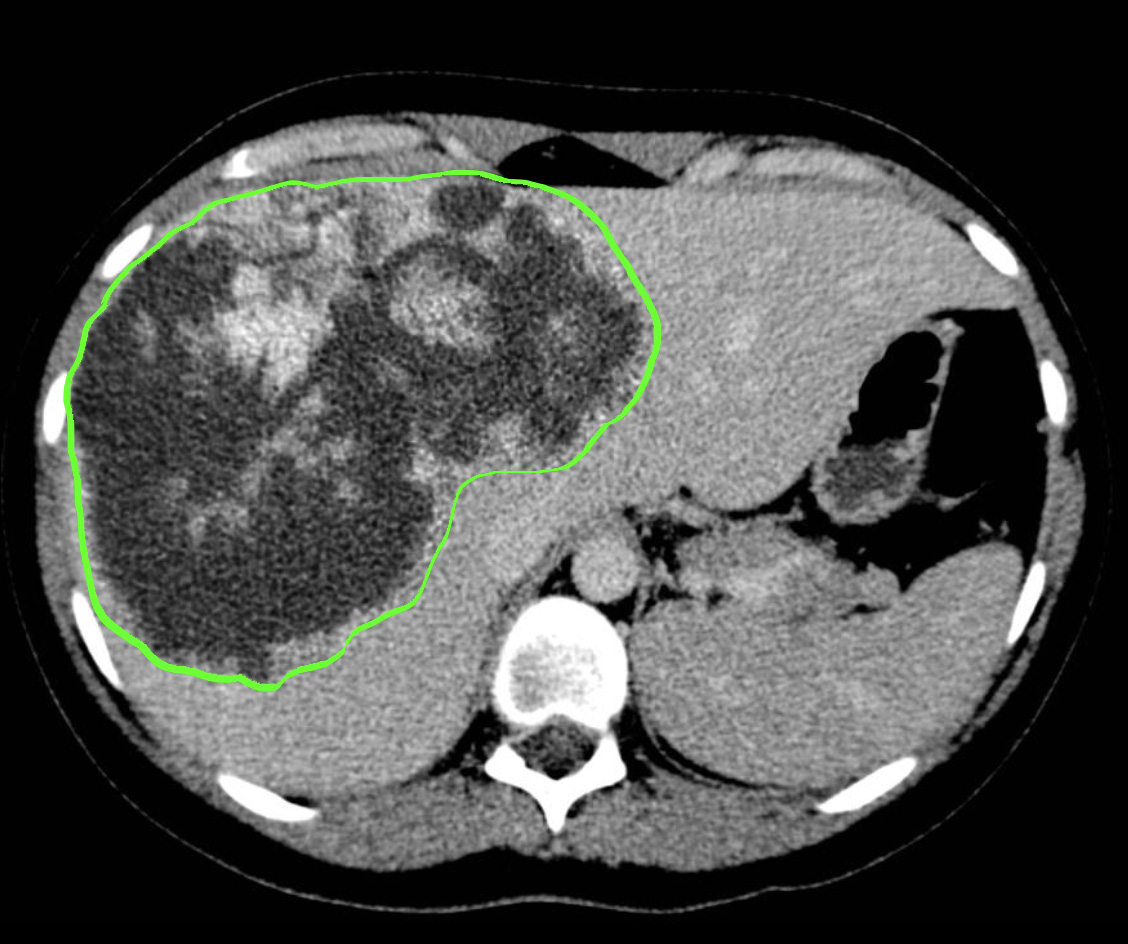
- Abdominal ultrasound or sonography
- Computed tomography scan (CT or CAT scan)
- Endoscopic retrograde cholangiopancreatography (ERCP)
- Esophagogastroduodenoscopy (also called EGD or upper endoscopy)
- Laparoscopy
- Liver biopsy
- Liver function tests
- Magnetic resonance cholangiopancreatography (MRCP)
- Magnetic Resonance Imaging (MRI)
- Percutaneous transhepatic cholangiography (PTC)
Liver Cancer Stages
When we diagnose liver cancer, the next step is to determine it stage, which indicates how advanced the cancer is and far is has spread. The National Cancer Institute defines the following stages for primary liver cancer:
Localized resectable (removable and operable)
Cancer is in the liver only, has not spread, and can be removed completely with surgery.
Localized unresectable (partially or fully inoperable)
Cancer is in the liver only, has not spread, but cannot be totally removed, usually due to its location near major blood vessels.
Advanced
Cancer has spread throughout the liver or to other parts of the body.
Liver Cancer Treatment Summary
Surgery
Surgery is a common method to remove the tumor from the liver. The operation to remove the cancer will likely include and a small portion of healthy liver tissue that surrounds the tumor. This is optimal if the tumor site is small, and the remaining part of the liver is in good health and functioning well.
Localized Treatment (Focused Ultrasound)
Histotripsy is a new type of treatment that uses focused ultrasound to destroy cancerous liver tumors. It can often eliminate tumors completely in a single treatment session, allowing patients can go home the same day after treatment. Other localized treatments may involve thermal (radiofrequency) ablation or cryoablation (extreme cold).
Radiation Therapy
Radiation therapy (or radiotherapy) is a medical treatment that uses high-powered energy rays such as X-rays or protons to destroy cancer cells and shrink tumors. Radiation therapy might be an option if other treatments aren’t possible or if they haven’t helped.
Chemotherapy
Chemotherapy uses drugs to kill rapidly growing cells, including cancer cells. Chemotherapy can be administered intravenously (through a vein), in pill form, or both. Advancements in chemotherapy can target specific parts of cancer cells, which provides very predictable results.
Embolization
Embolization is a procedure that injects substances directly into an artery in the liver to block or reduce the blood flow to a tumor in the liver.
Targeted drug therapy
Targeted drug treatments focus on specific abnormalities that are present within cancer cells. By focusing on these abnormalities, targeted drug treatments can block cancer progression and cause cancer cells to die.
Learn more
Click here for Liver Cancer Treatment.
Call today to learn more about Liver Cancer Diagnosis and Treatment. Our multi-disciplinary team is ready to support you.
If you have questions regarding Liver Cancer and symptoms, please call today. Click here to request an appointment.