What is Basal Cell Carcinoma?
Basal Cell Carcinoma (BCC) is the most common form of skin cancer, comprising about 1/3 of all new cancers. It manifests as an uncontrolled growth or lesion that arises in the skin’s basal cells, which line the deepest layer of the epidermis. Basal cell carcinoma cases are reviewed by a multi-disciplinary tumor board at the Saint John’s Cancer Institute to develop individualized treatment plans for patients treated at Saint John’s Health Center.
What Does Basal Cell Skin Cancer Look Like?
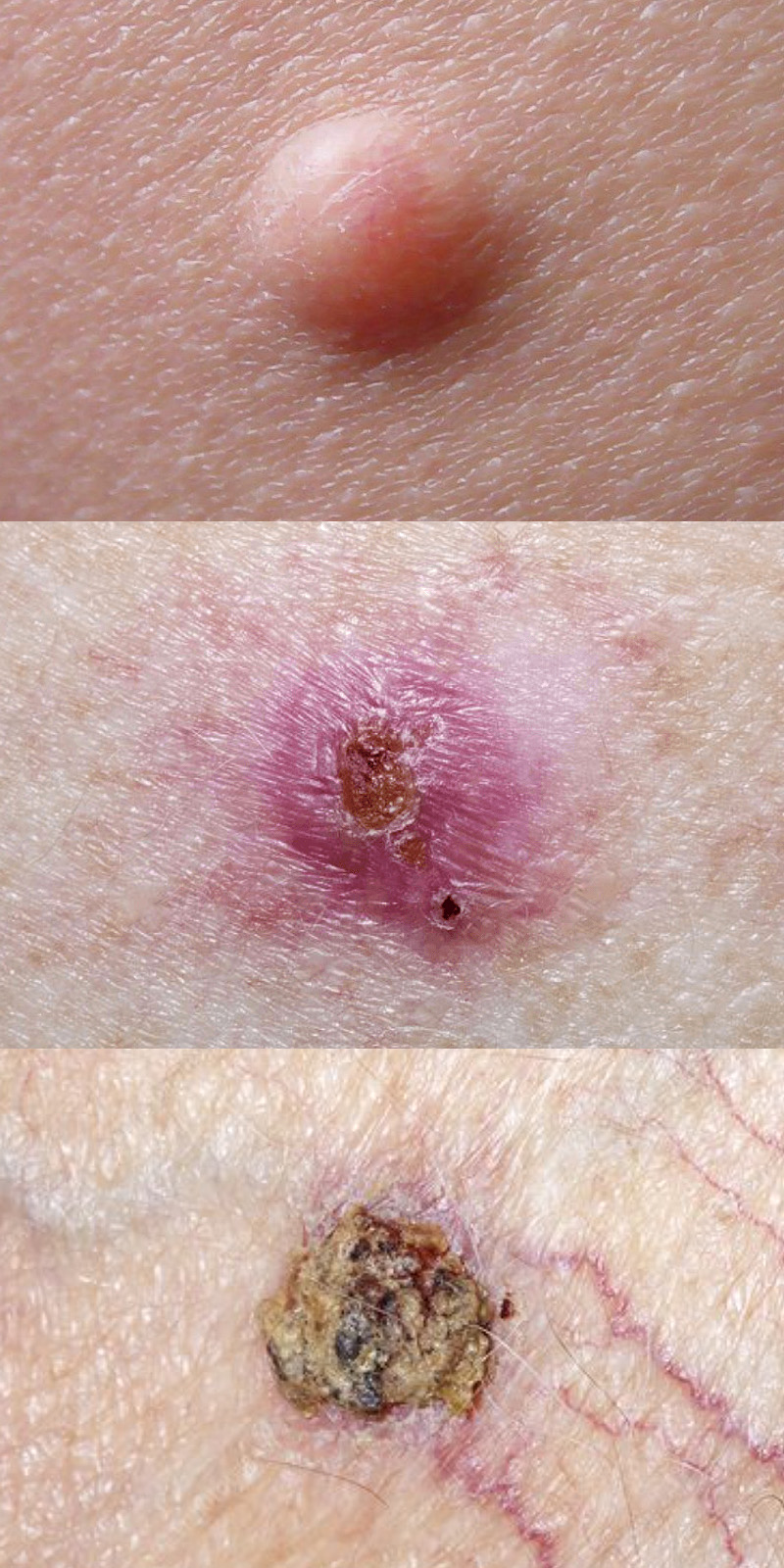
Basal cell carcinoma typically appears on sun-exposed areas of the skin, such as the face, neck, and hands. The appearance of basal cell carcinoma can vary, but there are some common characteristics of this type of skin cancer:
- Pearly or Waxy Bump: One of the most typical forms of BCC is a small, raised, translucent bump on the skin. The bump might be pearly or waxy in appearance, and it can have tiny visible blood vessels on the surface. This is often seen on the face.
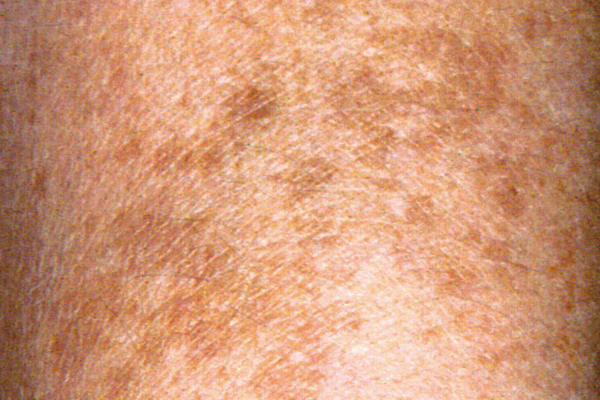
- Flat, Scaly Patch: BCC can also present as a flat, scaly, reddish patch. This type of BCC is more common on the trunk skin and can resemble eczema or psoriasis.
- Scar-like Area: Sometimes BCC appears as a white, waxy, scar-like area that is smooth and firm to the touch. This can be more difficult to identify because it might not look like a typical skin cancer.
- Sore that Bleeds, Oozes, or Doesn’t Heal: A common sign of BCC is a sore that bleeds, crusts over, and then reopens, or a sore on the skin that doesn’t heal over a few weeks.
- Pigmented Bump: In some cases, BCC can appear as a dark lesion on the skin, which might look like a mole or even melanoma. This type is more common in individuals with darker skin tones.
What Causes Basal Cell Carcinoma?
Basal Cell Carcinoma is usually caused by an accumulation of ultraviolet (UV) radiation exposure. Almost all BCCs occur on parts of the skin that receive the most sunlight, such as the face, scalp, ears, neck, shoulders, and back. Basal cell cancer on the scalp and nose is especially troublesome, with recurrences typically taking place within the first two years following surgery. Should a cancer recur, your physician might recommend a different type of treatment.
Only on rare occasions do they form on unexposed areas. Basal cell carcinoma occurs when one of the skin’s basal cells develops a mutation in its DNA. They can be highly disfiguring if allowed to grow, but they almost never metastasize (spread to other parts of the body) beyond their original location.
Though it is rare for basal cell carcinoma to metastasize, it is very likely for these cells to continue to grow.
Risk Factors for Basal Cell Carcinoma
Anyone with a history of sun exposure can develop basal cell carcinoma. It may take many years to reach accumulated exposure, which is why the disease is rarely seen in children. However, some teenagers are affected by skin cancer. In adults, men outnumber women in confirmed cases, but more younger women are getting BCCs today than in the past.
People who are at the highest risk have fair skin, blond or red hair, can freckle easily, and have blue, green, or grey eyes. Prolonged sun exposure or using tanning beds increases the risk of basal cell carcinoma. The threat is greater if you live in a sunny climate (Southern California) or a high-altitude city (Denver, Colorado), both of which expose you to more UV radiation than in other locations. Having severe sunburns also increases your risk of skin cancer.
Other factors that affect skin cancer
Sun exposure and the use of tanning beds do not explain all the cancers that develop on the skin. For example, radiation therapy can induce DNA mutations similar to those of natural sunlight. Therefore, radiation treatments are designed to reduce risk by limiting the radiation dose or giving fewer doses. Age is also a factor. Because basal cell carcinoma often takes decades to develop, most basal cell carcinomas occur in older adults. If you had basal cell carcinoma one or more times in the past, you have a good chance of developing it again.
A family history of skin cancer presents increased risk as well as certain immune-suppressing drugs. Medications used after transplant surgery, for example, can increase risk because they suppress the immune system. Exposure to toxins, such as arsenic, can also induce similar risk. In addition, certain rare genetic diseases can also increase the risk of basal cell carcinoma, including nevoid basal cell carcinoma syndrome (Gorlin-Goltz syndrome) and xeroderma pigmentosum.
Basal Cell Carcinoma Diagnosis & Treatment
When seeking care for basal cell carcinoma, the whole body is examined for lesions, not just the affected area. A skin biopsy may be performed for suspicious moles to determine if cancer is present and which cancer it is. The type of skin biopsy performed will depend on the type and size of the lesion.
A diagnosis of basal cell carcinoma can only be confirmed with a biopsy. This process involves taking a small piece of the affected tissue and examining it in our laboratory. Additional tests may be needed. If cancer cells are present, treatment is required. Fortunately, there are several effective methods available.
Treatment options are based on:
- Type of cancer
- Size of the tumorous tissue
- Location of the BCC
- Depth of the tumor (does it extend to the dermis and beyond)
- The patient’s age and general health
- The likely cosmetic outcome of specific treatments
In many cases, a simple excision (surgical removal) can be curative. A dermatologist might perform this. A technique called Mohs surgery may be performed to maximize skin preservation, which requires a surgeon specialist. In some cases, other treatments including radiation or topical therapies may be considered.
Surgery
Surgical excision of the affected tissue removes the cancerous lesion and a surrounding margin of healthy skin. This helps to reduce the risk of recurrence. The extent of the margin is determined by microscopic examination to verify the absence of cancer cells in the surrounding margin. Surgery is typical for basal cell carcinomas in areas that are less likely to recur.
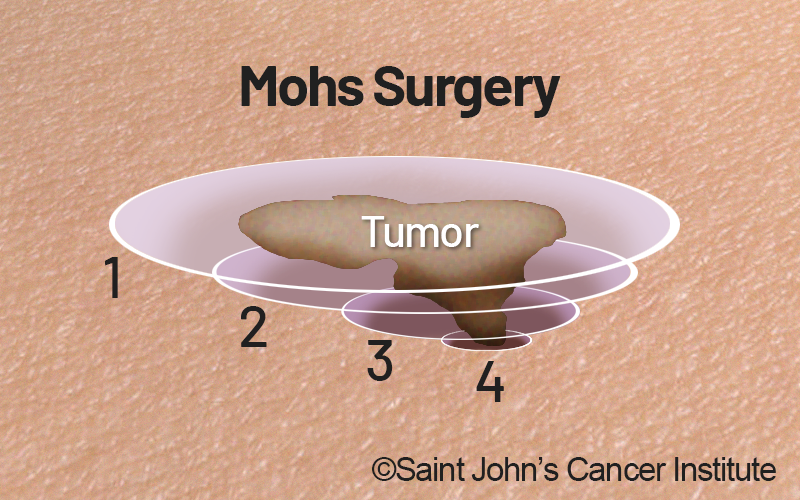
Mohs Surgery
Mohs surgery is a specific method of excision designed to conserve as much normal tissue as possible. During Mohs surgery, the cancer is removed layer by layer, which allows examination of each layer under a microscope until no abnormal cells remain. This guides the direction and depth of the surgery, thereby removing the entire growth while avoiding healthy skin. If your basal cell carcinoma is larger and has an elevated risk of recurring, extends deeper, or is located on your face, Mohs surgery may be the recommended treatment.
If you are unable to undergo surgery or if you have decided against having surgery, the oncologist may recommend other types of treatment.
Radiation therapy
Radiation therapy uses high-energy beams, such as X-rays and protons, that kill cancer cells by disrupting their DNA. By focusing the beams to the target area, the therapeutic result is maximized while reducing side effects. Radiation therapy can be given after surgery to help reduce the chance of recurrence and may be used when surgery is not an option.
Freezing (Cryosurgery)
Some cases of basal cell cancer can be treated entirely using liquid nitrogen, killing the cells by freezing them. This is particularly useful for treating smaller, superficial skin lesions, or when surgery is not an option. Freezing can also be combined with curettage treatment, which removes the surface of the skin cancer.
Topical treatments
Prescription creams and ointments are a viable option for small basal cell carcinomas that are less deep and when surgery is not an option. Like other prescription medicines, it is used as required by the treating physician.
Treatment for basal cell carcinoma that spreads
It is rare for basal cell carcinoma to spread (metastasize) to the lymph nodes and other areas of the body. If this occurs, however, there are treatments designed to help suppress cancer spread and its growth.
Targeted Therapy
Targeted drug therapy may be recommended by the oncologist and works by taking advantage of genetic and molecular flaws within cancer cells. By blocking the cancer’s ability to sustain itself, it shrinks and dies. Targeted therapy drugs may be considered after other treatments or when those treatments are not possible.
Chemotherapy
Chemotherapy drugs are designed to kill cancer cells. It might be an option when other treatments have not helped. Can be given orally, intravenously, or in other ways while doses are carefully selected to target the specific type and stage of the cancer.
How to Prevent Basal Cell Carcinoma
Chronic exposure to sunlight is one of the highest risk factors in the development of basal cell cancers.
Prevention methods include:
- Avoid the sun between 10 AM to 4 PM when UV radiation is the strongest.
- Avoid using tanning beds.
- Wear sun-protective clothing and hats to cover skin.
- Use a broad-spectrum sunscreen (30 SPF or greater) if outside for extended periods.
- See a dermatologist once a year for a head-to-toe skin examination.
For high-risk patients, research has shown that nicotinamide, a vitamin B3 supplement, reduced the rate of new squamous cell and basal cell skin cancers by approximately 23% compared with placebo.
If you have questions regarding basal cell carcinoma or other skins cancers, please call today or click here to schedule an appointment for an expert second opinion or click here to schedule an appointment.