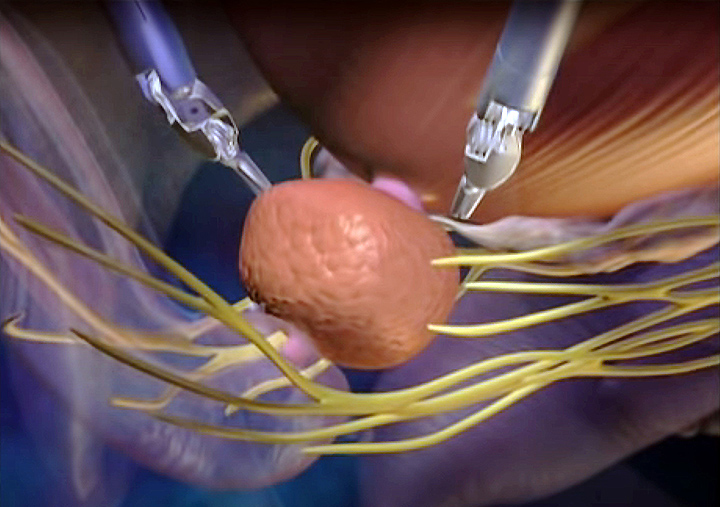
A Multidisciplinary Approach to Urology Care
 We are multidisciplinary team of urologists and urologic oncology experts who work with other specialists to provide the best clinical care possible. By involving other oncologists, including experts in radiation oncology, we ensure that our patients have access to greater treatment options, improved clinical outcomes, and answers to all their questions.
We are multidisciplinary team of urologists and urologic oncology experts who work with other specialists to provide the best clinical care possible. By involving other oncologists, including experts in radiation oncology, we ensure that our patients have access to greater treatment options, improved clinical outcomes, and answers to all their questions.
Once surgical treatment is completed, radiation may be the next step of your treatment. Radiation works to eliminate cancer cells at the tumor site that may remain after surgery, which is considered a supplement treatment. Radiation planning and treatment is provided at Saint John’s Health Center—a renowned, community-based, hospital in Santa Monica, California. We understand that your treatment is more than medical care, but a complete journey to wellness and improved quality of life.
Why use radiation therapy for urologic cancers?
Radiation therapy (or radiotherapy) works by disrupting the DNA of cancer cells. Where normal cells can recover after limited doses of radiation, cancer cells lose their ability to replicate, and as a result, shrink over time. Highly advanced imaging and tracking systems are involved with radiotherapy, ensuring that only the tumor site receives the therapeutic dose of radiation.
If radiation is recommended after surgery or prescribed with other treatments, its function is to reduce the likelihood of cancer spread by treating the immediate area where cancer is likely to recur. Radiotherapy can also be used as a primary treatment where more focused beams are used for curative intent, such as with small, well-defined tumors that are too difficult to remove surgically. The radiation oncologist works with radiation therapists—technicians who prepare the patient and equipment for radiation delivery, as well as physicists and dosimetrists—individuals who develop the radiation delivery models and dose distribution calculations according to the prescribed treatment.
Is radiation therapy for urologic cancers painless?
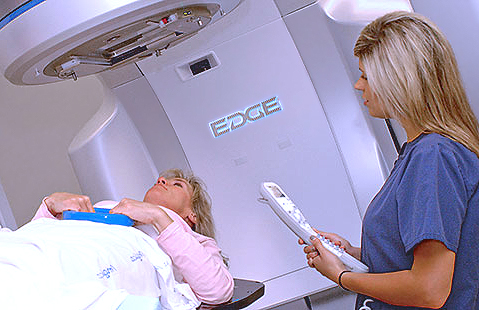
External beam radiation is a painless procedure, which usually takes 5 to 15 minutes. The number of treatments needed will vary for each person, the location of the cancer, and according to the technology used. In some cases, treatment may be daily and last for several weeks. Depending on the location of the tumor and the number of treatments, some patients may experience a condition that is similar to a sunburn on the surface of their skin, which is treated using topical medications. Radiation therapists prepare each patient for treatment, making sure they are comfortable and in the correct treatment position.
Newer treatment innovations have fostered more concentrated forms of radiation delivery, which results in fewer doses, or a single dose, instead of receiving many treatments over several weeks. Radiation can also be used to shrink a tumor before it is removed surgically, which reduces the amount of normal tissue that needs to be removed near the tumor. When cancer has spread, radiation therapy can also be combined with chemotherapy.
Innovation for Prostate Treatment – SpaceOAR™ Hydrogel
SpaceOAR™ Hydrogel is clinically proven to minimize urinary, sexual, and bowel side effects, while preserving the quality of life for prostate cancer patients undergoing radiation therapy. When treating prostate cancer patients with radiation therapy, the goal is to precisely target the treatment area while avoiding the healthy surrounding tissue.
SpaceOAR™ is an injectable gel that creates a small space between the rectum and the prostate, reducing the likelihood of the rectum being exposed to radiation treatment. SpaceOAR™ Hydrogel minimizes potential side effects of prostate cancer radiation therapy, so you can continue to thrive after prostate cancer treatment. It stays in place for about 3 months, maintaining the separation between the prostate and rectum. After 6 months, the hydrogel product is naturally absorbed into the body and removed from the urine.
Radiation Treatment Planning and Simulation
Radiation therapy is globally available and used to treat many types of cancers including lung, breast, prostate, and brain. In recent decades, advances in radiation physics and computer technology have made it possible to tailor the radiation beam and dose more precisely. Conformal Radiation Therapy (CRT), for example, uses CT images to precisely locate and map the treatment area in 3 dimensions, giving the radiation oncologist greater visibility and precision to deliver the most optimal treatment plans.
Every radiotherapy treatment is preceded by the development of a treatment plan. This process brings together the details of the entire treatment including imaging of the treatment area, identification of critical structures in the body, the dosing distribution, as well as the positioning of the patient and placement of small marks on the body for proper alignment. Treatment planning involves the radiation physicist and dosimetrist who collaborate to ensure effective radiation delivery and dose, while working to maximize curative effect, preserve healthy tissues, and minimize the potential for side effects.
Treatment Simulation
After the treatment plan is developed, a treatment simulation is performed. The simulation is like a radiation treatment test run, which allows the care team to replicate all the motions of treatment without delivering any radiation. The radiation therapists are responsible for performing treatment simulation and treatment delivery, which includes preparing the patient for treatment, helping them into the required treatment position, and aligning the small marks placed on the skin to visual guides projected in the room. Though treatment is delivered from a control console outside of the radiation delivery room, the radiation therapists can always communicate with the patient during treatment.
If you have questions regarding treatments for urologic cancers and conditions, please call today. Click here to request an appointment.

Providence St. John’s Health Center
High Performing in Urology
High Performing in Urology
Saint John’s Health Center is nationally ranked and in the top 10% for Urology
Learn more at Health.USNews.com.