If you have questions regarding Ureteral Cancer treatment, please call today. Click here to request an appointment.
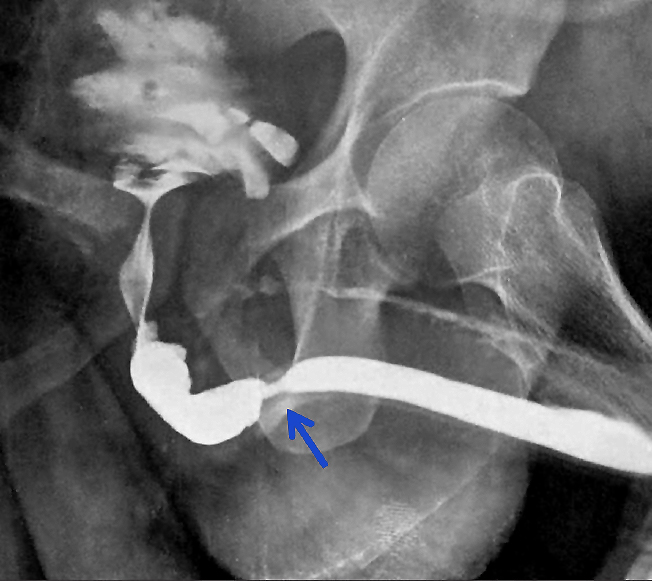
Ureteral Cancer and Upper Tract Urothelial Carcinoma (UTUC)
Ureteral Cancer and Upper Tract Urothelial Carcinoma (UTUC)
Schedule An Appointment
Saint John's: Our urology program is nationally recognized and awarded, including High Performing in Urology, and the George M. Drach Award