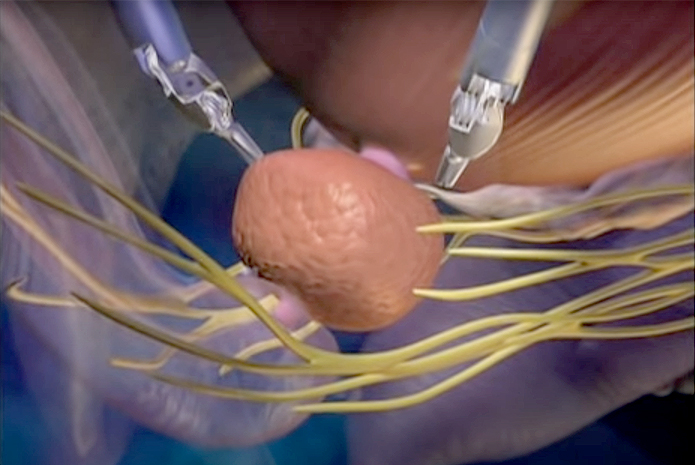
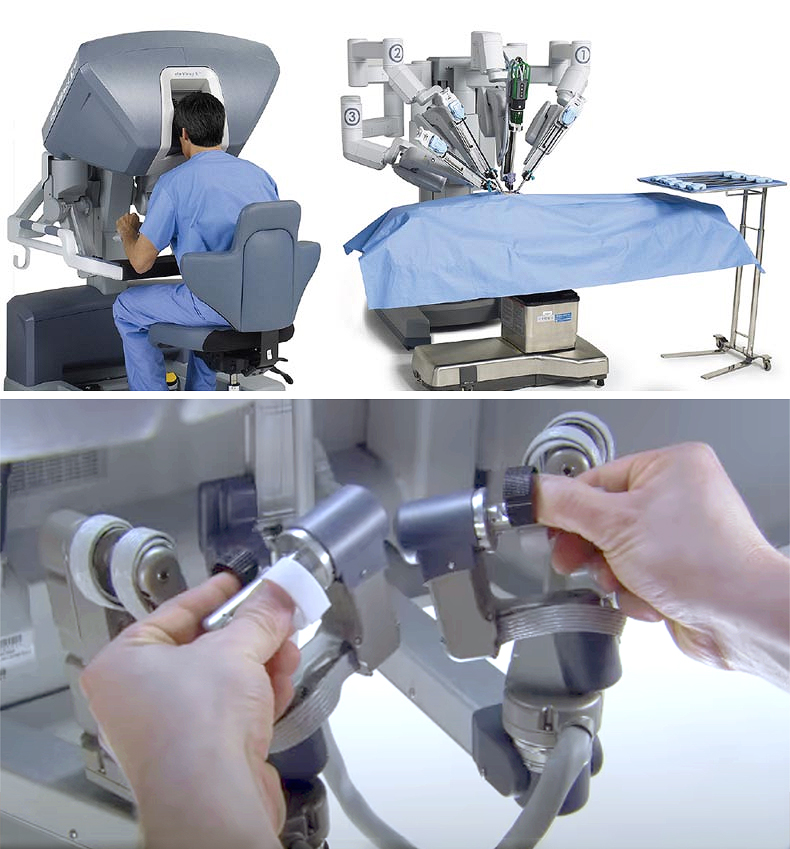
What is Robotic Prostate Cancer Surgery?
Robotic Prostate Cancer Surgery is a technology innovation that extends the ability of the urologist. He or she may have the experience and skill to conduct the surgery without robotics but can now perform more detailed movements in a much smaller space. This assisted procedure helps to reduce hospital stays and recovery time. Though prostate cancer can be treated in a variety of ways, some patients with more advanced cancer may choose surgery.
Robotic Prostate Cancer Surgery may be the best option for improved outcomes. During the procedure, the surgeon is seated at a console near the patient but not directly at the patient’s side. An assistant, who is also a doctor, is positioned with the patient the entire time. The operating surgeon controls the robotic instruments while the robot reproduces the surgeon’s sophisticated maneuvers precisely.
Why Remove the Prostate?
Sometimes it may be best to remove a cancerous prostate gland entirely. This is referred to as complete or radical prostatectomy. It is a minimally invasive procedure that has become more efficient and precise with the use of robotics. Men can live normal lives without the prostate gland.
Our goal is to guide you or your family member through the entire treatment process, helping you to understand the procedure and ultimately beat the cancer, while working to retain as much normal function as possible. Dr. Timothy Wilson and his team of urologic and radiation oncologists have decades of experience treating thousands of prostate patients successfully.
Will I Retain the Function that I Have?
Men tend to recover physically more quickly, allowing them to resume their normal activities in just a few weeks. They also tend to regain bladder control and sexual function more readily simply by staying physically active. This helps to improve recovery. Subtle modifications in the procedure are tailored to the individual patient depending on the details of their cancer. However, a robotic-assisted radical prostatectomy allows the surgeon to do a more accurate and reliable procedure which improves patient outcomes and quality of life.
Our Primary Goal is Cancer Cure
Overcoming cancer is our goal. Secondary goals, which also critically important, include speedy physical recovery, continence recovery, and erection recovery. Statistically, 10% of men can have an erection that supports intercourse within six weeks following surgery. About 50% of men reach this level of function at six months and about 85% will achieve normal function at one year. Recovery of erections is affected by the level of function before the surgery, age of the patient, the presence of other medical problems like diabetes and high blood pressure, while smoking, alcohol intake, stress, your partner, and a few other things are also a factor. In short, it is complicated.
Research suggests that a single dose of generic Viagra (sildenafil citrate) or Cialis (tadalafil) taken a few days before surgery may lessen the shock to the sexual function nerves as they are carefully separated from the prostate. In addition, research also suggests that taking such medications (generic or brand name products) after surgery daily may help nerve recovery. It is important to know that if the nerves are disturbed, drugs for erectile dysfunction will not “make an erection,” however, by taking them daily, it may help promote a rapid and more complete erection recovery. Your surgeon and care team will discuss this in detail before and after surgery. In addition, other methods are used to keep the penis in good health while the sexual function nerves begin to “wake up.” These methods include things like vacuum erection devices (medically approved penile pumps), injection therapy, testosterone replacement therapy, and shockwave therapy.
Benefits of Robotic Surgery for Prostate Cancer
By using the surgical robot, the surgeon has improved visualization of the prostate and surrounding structures, which allows for a more precise surgery. In all cases, the biopsy details of the prostate, along with Magnetic Resonance Imaging (MRI), are used to guide the surgery. This allows for a more consistent, reliable, and reproducible operation.

Outcomes and clinical benefits include:
- Same cancer cure rate as traditional surgery
- Shortened physical recovery
- Highest cure rates compared to other treatments
- Improved functional recovery of bladder control and sexual function
- Best possible way to know the full extent of the cancer
- Assessment of local/regional lymph nodes to check for cancer spread
What to expect during and after prostate cancer surgery
At the time of surgery, patients will have a urinary foley catheter placed in the urethra. Upon hospital discharge, patients will keep the urinary catheter with them for one week. Urine drains into a small bag that is strapped to the upper leg. There is a valve at the bottom of the bag to empty it from time to time. It will be necessary to drain the bag as it fills.
After the surgery and while still in the hospital, patients will begin digesting clear liquids. This will be followed by solid food based on the surgeon’s recommendations. The first bowel movement occurs three to four days later, which is normal. In order to make the first bowel movement as easy as possible, we recommend drinking prune juice daily, while taking a stool softener and laxative. These are highly important to consider because patients should minimize straining and pushing during a bowel movement after treatment.
Showering is OK the day after surgery. In some patients, the urinary catheter may irritate the tip of the penis. A small amount of antibiotic ointment, such as Bacitracin or Neosporin ointment, applied after showering, can relieve this irritation. This is available over the counter in most pharmacies.
Your Prostate Surgery Recovery and Follow-Up
Although rest after the surgery is important for healing, walking is just as important. Resting too long can adversely affect the way you feel and may prolong the healing process. If you were very active before your surgery, you will probably want to resume your regular routine as soon as possible. If you were only moderately active before surgery, it is still important to become active. Be sure to start slowly with more gradual, gentle exercises. Walking is the best way to get back to feeling normal again. We recommend patients take a 10–15-minute walk three times a day if possible. You may resume sexual activity per your doctor’s instruction. There are a few restrictions after surgery:
- No lifting more than 15 pounds for at least six weeks
- No bicycle riding, horseback riding, or motorcycle riding for two months
- Use common sense (If it hurts, don’t do it)
Before being discharged from the hospital, you will receive instructions from your nurse and doctor regarding diet, physical activity, and care of the urinary catheter. About one week after discharge, you may be asked to return for a post-op checkup and X-ray. During this visit, it is likely that the catheter will be removed by the nurse, while the doctor checks on your recovery progress. The physician will also review the pathology (biopsy) report of the tissue that was removed during the prostate cancer surgery.
Subsequent follow-up visits with your doctor are needed about every three months for the first year then every six months after the first year. At each follow-up visit, a blood test is performed to measure PSA (Prostate Specific Antigen) in the blood. PSA is a protein produced by normal cells in the prostate and by prostate cancer cells. After surgery, the PSA outcome should be ‘non-detectable’—a determination that reveals we did not find any PSA. The urologist will assess overall health, bladder function, and sexual function during the follow-up visit.
Stage 4 prostate cancer survivor explains his recovery after robotic prostate cancer surgery
Stage 4 Prostate Cancer—a story of inspiration and strength told by survivor, Dan Garr.
Risks of Robotic-Assisted Prostatectomy
Robotic prostate surgery can have two main risks—incontinence and impotence. The degree of sexual function after surgery is directly related to the patient’s sexual function prior to the surgery. The surgeon uses enhanced visualization through the robotic system to better see the nerves around the prostate which helps the doctor avoid these sensitive structures, thereby retaining optimal function after the surgery. Prostatectomy is the removal of the entire prostate gland.
Urinary Continence Recovery
It is common for men to have some leakage of urine (urinary incontinence) following prostatectomy. This is temporary and commonly resolves within six weeks. During recovery, men should perform pelvic floor exercises, such as Kegel exercises, to help resolve urinary leakage. If bladder control is slow to recover, physical therapy and medications can help improve function. If the problem persists, a minor surgical procedure can typically resolve the problem. This sort of procedure is needed in only 1 to 2% of men after prostatectomy. It is important to know that most men will return to normal urination within a few months while erectile function may take longer.
Sexual Function Recovery
Important principles regarding recovery of sexual function:
- Having a prostatectomy does not affect the way that you think about sex.
- Having a prostatectomy does not affect sensation of the penis (the way it feels to touch).
- Having a prostatectomy does not affect your testosterone level – though many men above the age of 40 begin to develop lower levels of testosterone naturally.
- Having a prostatectomy does not affect your ability to experience a sexual climax (orgasm). This usually returns in over 90% of men within one month. In addition, the quality of the climax rarely diminishes (about 5% of the time) but the sensation may be somewhat different.
- Because we are removing the organ that makes semen, it will no longer be produced after a prostatectomy. This is evident during male climax. This is also true for most men that have radiation as a treatment.

The objective of prostatectomy surgery is to spare the nerves that travel along each side of the prostate, so long as it is safe to do so from a curative perspective. Unfortunately, cancer can involve these nerve bundles as well. Many techniques have been developed over the last 20 years that promote nerve recovery, which is an active part of our clinical program. We make every attempt to use these techniques during prostatectomy.
Other side effects
Swelling
Some patients will have swelling in the penis and in the scrotum. Swelling of the penis and scrotum is normal after prostate surgery and will eventually resolve with time, though it may take a few weeks. If your penis or scrotum is swollen, you may wear a compression garment to aid in the recovery.
Infection
Infection is rare following surgery but can happen within the superficial wounds of the skin or from deep inside. The urology team will monitor your recovery and signs or symptoms of infection.
Hernia
Hernias of the abdominal wall related to the incisions can occur after any surgery. To minimize this risk, we ask patients to avoid heavy lifting above 15 pounds or physical straining for at least six weeks after surgery.
Blood Clots – Deep Vein Thrombosis (DVT)
Blood clots after this surgery are very uncommon but do occur. To help prevent this problem, we use special prophylactic compressors (leg squeezers) during and after surgery. We also, have the patient begin walking within 8 to 12 hours after the surgery.
Bleeding
Some bleeding can occur after a prostatectomy, which is common with any surgery. Robotic surgery is a form of laparoscopic surgery, which by its nature, results in smaller incisions and less blood loss. The number of men requiring blood transfusion during or after robotic prostatectomy is less than 1%. We do not ask men to donate their own blood prior to surgery because we have blood available that has been screened specifically for each patient and available if needed.
Injury to Neighboring Organs
Injury to nearby organs, such as the intestine, blood vessels, and ureters, can happen during this kind of surgery. However, the physicians at Providence Saint John’s Health Center are highly experienced and so these kinds of events are extraordinarily rare. However, should they occur, we are always prepared to manage them effectively, resolving them in the best possible way to minimize any impact to your recovery.
Other Complications
As with many things in life, the unexpected can occur. Fortunately, modern medicine and extensive surgery training prepares us for the unexpected. At the Providence Saint John’s Health Center, we have access to experts in a broad range of medical specialties and are 100% confident that we can address problems and unforeseen complications effectively. Our goal, of course, is to provide the highest level of medical and surgical care that promotes the best possible recovery for each patient.
We are Ready to Support You
Like many surgeries for cancer, this is a life-changing procedure that changes how the body functions. It is normal to experience some changes in the way you see your body and the way you feel. There are many resources that are available to help you cope with the way you feel and how to cope with these changes.
Call our office today and learn more about this innovative procedure and all of our highly experienced Urologists. We have treated thousands of patients using robotic surgery, which has helped to improve clinical outcomes and promote quality of life for our patients.
Click here to request additional information or to make an appointment.
If you have questions regarding treatments for urologic cancers and conditions, please call today.
About the da Vinci Robotic System and Assisted Surgery
The da Vinci surgical system is operated by a surgeon, allowing them to successfully perform a complex, yet non-invasive surgical procedure. Through a small incision, the surgeon uses delicate instruments, a magnifying camera and lighting. Since the procedure is performed using a smaller opening, there is a reduced chance of bleeding than with traditional surgery. Comparing the da Vinci robotic system to traditional surgery, much smaller scars result, which may further reduce the risk of an infection because the incisions are smaller. The da Vinci robotic system is also used in gynecologic, head and neck, cardiothoracic medicine, and general surgery.
Robotic surgery was approved by the FDA for prostate cancer treatment (Robot-Assisted Radical Prostatectomy – RARP) in 2001. Initially, there were concerns that this technique of surgery may lead to higher cancer recurrence rates or higher complications. However, many countries that use robotic surgery share their experiences, which contributes to even greater best practices guidelines in support of optimal outcomes. This data reveals conclusively that robotic surgery does not compromise cancer control rates, which are applicable to all risk groups.

Providence St. John’s Health Center
High Performing in Urology
High Performing in Urology
Saint John’s Health Center is nationally ranked and in the top 10% for Urology
Learn more at Health.USNews.com.