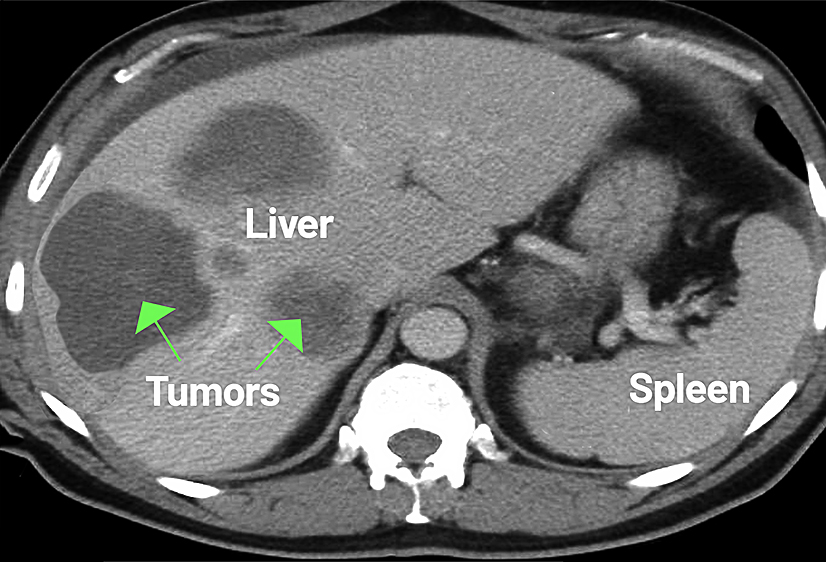
Adrenal cancer is a rare condition that affects the adrenal glands—two small organs located above the kidneys that produce essential hormones. While many adrenal tumors are benign, adrenocortical carcinoma (ACC) is an aggressive form of adrenal cancer that requires experienced, multidisciplinary care.

At the Center for Endocrine Tumors and Disorders, at Saint John’s Cancer Institute, we combine decades of oncologic research, medical advancements, and surgical expertise with compassionate, personalized care for our patients at Saint John’s Health Center, in Santa Monica, CA.
Understanding Adrenal Cancer and Adrenal Gland Tumors
Most adrenal tumors are noncancerous, but some may produce excess hormones or become malignant. The primary types of adrenal cancers include:
- Adrenocortical carcinoma (ACC): A rare cancer arising from the adrenal cortex (outer layer).
- Pheochromocytoma and neuroendocrine tumors: Tumors originating from hormone-producing cells in the adrenal medulla (inner portion).
The most common malignancy involving the adrenal gland is actually metastatic adrenal cancer, where cancer spreads from another organ—such as the lung, breast, kidney, gastrointestinal tract, or skin—to the adrenal gland.
Although ACC is rare, early diagnosis and timely treatment can significantly improve outcomes. It is more frequently diagnosed in children under age 10 and adults over age 50.
Symptoms of Adrenal Cancer and Metastases
Symptoms depend on whether the tumor produces excess hormones or grows large enough to affect surrounding structures.
Hormone‑Related Symptoms
- High blood pressure
- Diabetes
- Round, full face (“moon facies”)
- Fat accumulation on the upper back (“buffalo hump”)
- Stretch marks on the abdomen or thighs
- Abnormal hair growth (hirsutism)
- Irregular menstrual cycles

General Symptoms
- Easy bruising
- Fatigue or weakness
- Unexplained weight gain
- Leg swelling or muscle cramps
- Mood changes or irritability
- Muscle weakness
- Back or abdominal pain from a large tumor
If you are experiencing persistent or unexplained symptoms, evaluation by an adrenal specialist or endocrinologist is recommended.
Risk Factors for Adrenal Cancer
Most cases of ACC occur without a known cause. However, certain rare genetic syndromes increase risk, including:
- Li‑Fraumeni syndrome
- Lynch syndrome
- Beckwith‑Wiedemann syndrome
A family history of endocrine cancers or inherited tumor syndromes may also increase risk.
Metastatic adrenal cancer most often originates from primary cancers of the lung, breast, kidney, or gastrointestinal tract.
For individuals with a family history of endocrine disorders or known genetic risk, our genetics team provides counseling and screening to support early detection.
Diagnostic Tests for Adrenal Cancer and Metastases
Accurate diagnosis is essential for determining the most effective treatment plan. Our team uses advanced imaging and hormone testing to evaluate adrenal tumors.
Hormone Testing
Hormone testing plays a central role in evaluating adrenal tumors, as many adrenal cancers produce excess hormones that cause noticeable symptoms. Blood and urine tests help measure levels of cortisol, aldosterone, and androgens, providing important clues about whether a tumor is functioning or non‑functioning. These results guide both diagnosis and treatment planning, ensuring that hormone‑related symptoms are properly managed throughout care.
- Blood and urine tests to measure cortisol, aldosterone, and androgen levels
- Evaluation for hormone‑producing tumors
Imaging Studies
Advanced imaging is essential for assessing adrenal tumors and determining whether cancer has spread beyond the adrenal gland. CT scans, MRI, and PET imaging help evaluate tumor size, shape, and involvement of nearby structures, offering critical information for surgical planning. Certain imaging features can also help distinguish benign adrenal masses from those that are more suspicious for adrenocortical carcinoma.
- CT scan
- MRI
- PET scan
Imaging helps determine tumor size, involvement of nearby structures, and whether the cancer has spread.
Biopsy Considerations
Biopsy is used selectively in the evaluation of adrenal tumors because, in some cases, it can pose risks or provide limited diagnostic value. When a tumor is suspected to be metastatic and hormone excess has been ruled out, a biopsy may help confirm the origin of the cancer. However, for suspected adrenocortical carcinoma, diagnosis is typically made after surgical removal, when a full pathology review can be performed safely and accurately.
Treatment of Adrenal Cancer
Treatment is tailored to each patient and may include surgery, medication, radiation therapy, or participation in clinical trials. Our endocrine surgeons and oncology specialists work together to develop a personalized plan based on tumor type, size, and stage.
Surgery (Adrenalectomy)
Surgery is the primary treatment for localized adrenal cancer. An open adrenalectomy removes the adrenal gland and, when necessary, surrounding tissues and lymph nodes.
Our surgical team, including Dr. Melanie Goldfarb, specializes in advanced adrenal surgery and en‑bloc tumor removal when appropriate.
Adjuvant Therapy
Adjuvant therapy may be recommended after surgery to reduce the risk of cancer recurrence, particularly in cases of adrenocortical carcinoma. Mitotane, a medication that specifically targets ACC cells, is often used as part of this approach. Depending on the tumor’s characteristics, chemotherapy or radiation therapy may also be incorporated to provide additional control and support long‑term outcomes. This includes:
- Mitotane therapy (targets ACC cells)
- Chemotherapy
- Radiation therapy
Unresectable or Metastatic Adrenal Cancer
When adrenal cancer cannot be removed surgically, treatment focuses on slowing disease progression and managing symptoms to maintain quality of life. Options may include mitotane therapy, combination chemotherapy, or participation in clinical trials evaluating new targeted or biologic therapies. Radiation therapy may also be used to control tumor growth or relieve pain, depending on the location and extent of disease. Options may include:
- Mitotane and combination chemotherapy
- Targeted therapies or biologic agents through clinical trials
- Radiation therapy for local control or pain relief
Prognosis and Follow‑Up Care
Adrenocortical Carcinoma Prognosis
Prognosis for ACC varies depending on the stage at diagnosis, the tumor’s biological behavior, and the success of surgical removal. Early‑stage tumors that can be completely resected offer the best chance for long‑term survival. Because ACC can behave aggressively, ongoing research and clinical trials continue to explore new therapies aimed at improving outcomes for patients with advanced disease. Prognosis depends on:
- Tumor size and stage
- Completeness of surgical removal
- Tumor biology and hormone secretion
Recurrence and Monitoring
Long‑term monitoring is essential for patients treated for adrenal cancer, as recurrence can occur months or even years after initial therapy. Follow‑up typically includes periodic imaging, hormone testing, and physical examinations to detect any signs of returning disease as early as possible. Our team works closely with patients to create a personalized surveillance plan that supports both medical needs and overall well‑being. Monitoring typically includes:
- Routine imaging studies
- Hormonal testing
- Regular physical examinations
Patients are followed by a multidisciplinary team—including endocrine surgeons, endocrinologists, and oncologists—to ensure early detection of recurrence and management of long‑term effects.
Innovations in Adrenal Cancer Treatment
Precision Medicine and Genomic Testing
Genomic testing provides valuable insight into the molecular characteristics of adrenal tumors, helping physicians identify specific genetic mutations that may influence treatment decisions. By understanding the tumor’s genetic profile, our team can determine whether targeted therapies or immunotherapies may be appropriate. This approach also helps identify patients who may benefit from participation in clinical trials exploring new and emerging treatments for adrenal cancer.
Multidisciplinary Endocrine Care
Our multidisciplinary model brings together experts in surgical oncology, endocrinology, medical oncology, and radiation oncology to ensure each patient receives coordinated, comprehensive care. This collaborative approach allows us to evaluate every aspect of a patient’s condition—from hormone balance to tumor behavior—so we can develop a treatment plan tailored to their unique needs. By working closely across specialties, we aim to improve outcomes while supporting long‑term health and quality of life.
Living with Adrenal Cancer

A diagnosis of adrenal cancer can be overwhelming. Our team provides support services—including nutritional counseling, symptom management, and survivorship programs—to help patients maintain their health and well‑being throughout treatment and recovery.
Emotional and psychological support is an important part of healing, and our programs help patients and families navigate the challenges of living with adrenal cancer.
Our team includes board‑certified endocrine surgeons, oncologists, and endocrinologists who specialize in adrenal cancer and complex endocrine tumors. We are ready to support you throughout your entire journey.
If you have questions regarding adrenal cancer, symptoms or treatment, please call today. Click here to request an appointment.