If you have questions regarding RFA treatments for benign thyroid nodules, please call today. Request an appointment
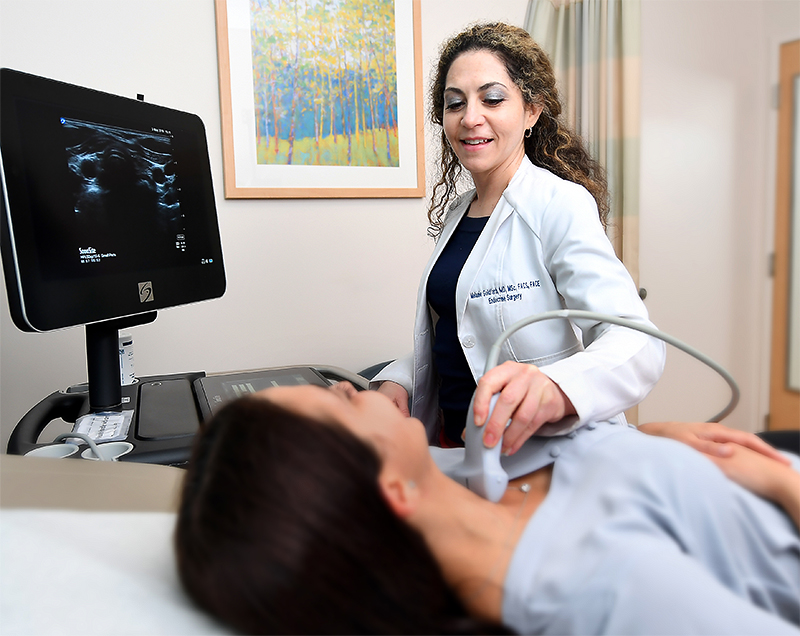
Melanie Goldfarb, M.D., M.Sc., FACS, FACE
Director, Center for Endocrine Tumors and Disorders
Medical Director for Cancer Survivorship
Dr. Melanie Goldfarb is a fellowship-trained endocrine surgeon and Director of the Center for Endocrine Tumors and Disorders. Her expertise is minimally invasive surgery for thyroid cancer and disorders, hyperparathyroidism, and adrenal tumors, including pheochromocytoma, Cushings, Conns, and adrenal cancer.
- Learn more about Dr. Melanie Goldfarb and access videos of patients who received RFA treatment.
- Meet the Endocrine Team
- Listen to a recent webinar on Radiofrequency Ablation (RFA) with Dr. Melanie Goldfarb.