If you have questions regarding Pheochromocytoma & Paraganglioma, or other endocrine conditions, please call today. Request an appointment
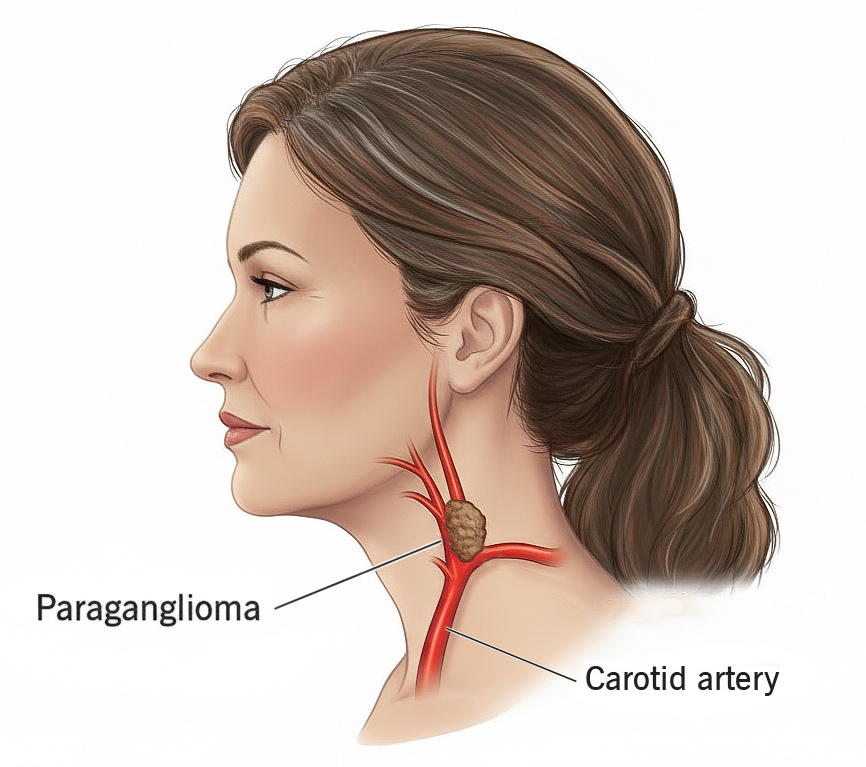
Pheochromocytoma & Paraganglioma
Pheochromocytoma & Paraganglioma
Schedule An Appointment
Saint John's: A Legacy of Care Excellence - 30 Major Healthcare Awards for 2022 and 2023