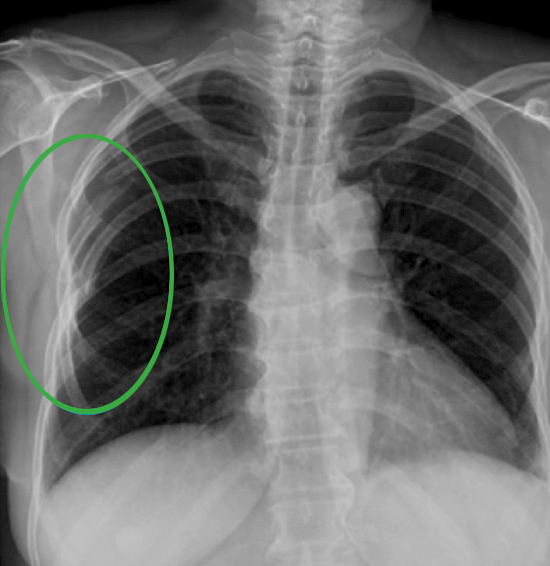
What are Chest Wall Conditions?
Chest wall conditions encompass a diverse range of medical disorders affecting the structural integrity of the chest wall. Among them, three significant categories are chest wall tumors, chest wall infections, and chest wall deformities (including rib fractures). Diagnosing these conditions typically involves a thorough medical history, physical examination, and advanced imaging techniques such as X-rays, CT scans, or MRIs.
Treatment approaches vary depending on the specific condition, with options ranging from conservative management, antibiotic therapy, and physical therapy to surgical interventions for more severe cases. Saint John’s Health Center aims to alleviate symptoms, restore chest wall integrity, and improve overall quality of life.
Chest Wall Tumors
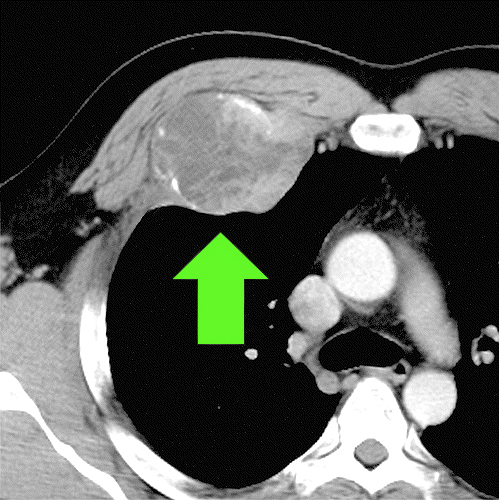
Like any other part of the body, the walls of the chest cavity are susceptible to tumors. A tumor is any type of abnormal growth of cells, whether malignant (cancerous) or benign (non-cancerous). Chest wall tumors can interfere with pulmonary function (breathing and/or circulation). While hereditary factors, diet, and lifestyle choices may play a role in certain tumor types, there are no clear causes of chest wall tumors.
Cancerous tumors are uncommon. Chest wall tumors, whether malignant are classified as primary or secondary (metastatic). The most common benign tumors are osteochondromas and chrondromas. The most common malignant chest wall tumors are sarcomas.
Primary tumors originate in the bone or muscle of the chest wall. Less than half of malignant chest wall tumors are primary. Secondary tumors originate elsewhere in the body and spread (metastasize) to the chest wall. Almost all secondary tumors are malignant. Most chest wall tumors found in children are primary, while most found in adults are secondary. All of these tumors tend to be a lump on the chest wall surface or a growth that invades the bone or muscle.
What are the Symptoms of a Tumor in your Chest?
- A localized mass
- Swelling
- Chest Pain
- Muscle atrophy (breakdown)
Symptoms of malignant (cancerous) chest wall tumors may include one or more of the following:
- A localized mass
- Swelling
- Chest Pain
- Impaired movement or chest expansion
Tests and Diagnosis
At Saint John’s Health Center, we will perform an X-ray to see if there is an abnormality. If there is an abnormality visible on the X-ray, we will do a CT scan (computed tomography) or MRI (magnetic resonance imaging) scan to gain additional information about the chest wall abnormality, such as size and location. These scans provide additional detail including soft tissue structures.
Biopsy
After this information is collected, a biopsy of the abnormality is obtained to diagnose what the tumor is and to determine if the tumor is cancerous. The most common procedure is an aspiration biopsy, in which a needle is inserted into the tumor cells are removed for examination. If it is too difficult to reach the tumor site, you may be asked to undergo an open biopsy, which requires a small surgical incision.

Treatment of Chest Wall Tumors
If the tumor is benign, the tumor may need to be surgically removed if it interferes with organ function such as breathing, causes pain, hinders movement, or causes muscles to atrophy. If the tumor is malignant, treatment can include a combination of chemotherapy, radiation therapy, and surgical removal and reconstruction.
It is typical for a portion of the rib cage to be removed to access the chest wall tumor. This is followed by reconstruction of the affected chest wall portion, which can include adjacent muscle or synthetic materials. The amount of chest wall that must be removed and the associated risks and benefits of the operation are reviewed with you and the surgeon before the procedure.
For additional information on Chest Wall Tumors treatment, click here.
Chest Wall Infections
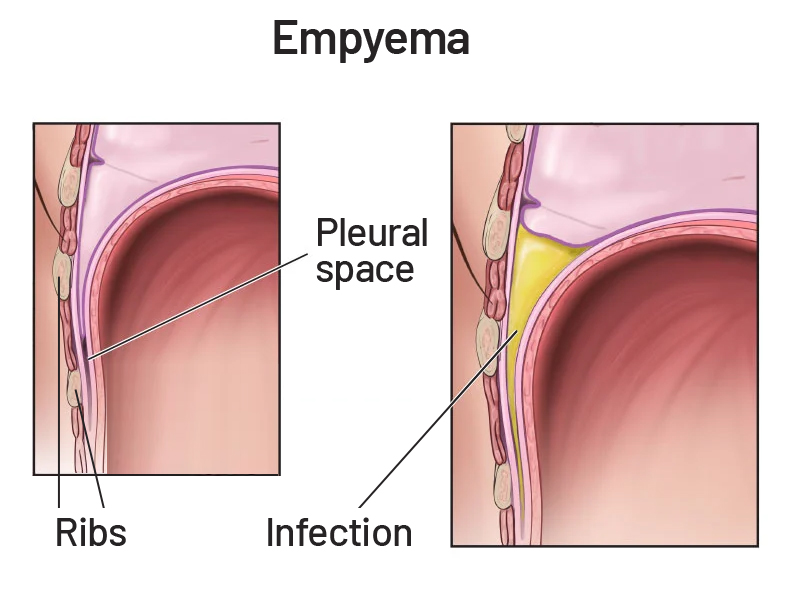
The chest wall is made up of the ribs, the sternum, and cartilage. Occasionally, infections of the chest wall might appear to only involve the skin but may represent a deeper infection of the ribs, cartilage, or other structures. An example of a chest wall infection is empyema—a fluid that collects in between the chest wall membranes (pleura) and the chest wall.
The reason for chest wall infections has various causes, including infections that can occur after a surgical procedure or secondary infections, which are infections that have spread to the chest wall from another part of the body.
Examples of secondary infections, causes, or risk factors include having:
- Pneumonia
- Trauma or injury to the chest wall
- Tuberculosis
Chest wall infections may also manifest in various ways, such as Pleuritis—an infection of the chest wall membranes (pleura). Costochondritis is another condition that involves inflammation of the chest wall cartilage which connects the ribs to the sternum (the breastbone). Bacteria, viruses, and fungi can also infect the chest wall, resulting in chest wall pain and inflammation.
Symptoms of Chest Wall Infections
The most common presenting symptom of a chest wall infection is chest pain. Chest pain may increase with activity or worsening of the infection. Other symptoms include
- Chest tenderness and swelling
- Pain when taking a deep breath
- Fever
- Dry cough
Diagnosis and Treatment of Chest Wall Infections
Possible diagnostic tests may include:
- Blood tests can help diagnose an infection.
- Chest X-rays
- CT scans may be used to identify inflammation in areas of the chest.
- Ultrasound Imaging
- Electrocardiogram (EKG) may help to rule out heart problems as a cause of your chest pain.
- Bronchoscopy may be used on chest wall tissues or the airway to look for signs of infection.
Chest wall infections are often treated with antibiotics and anti-inflammatory medications. However, certain chest wall infections may require surgery to remove the infection, along with possible reconstruction of the chest wall.
Chest Wall Deformity (Pectus Excavatum)?
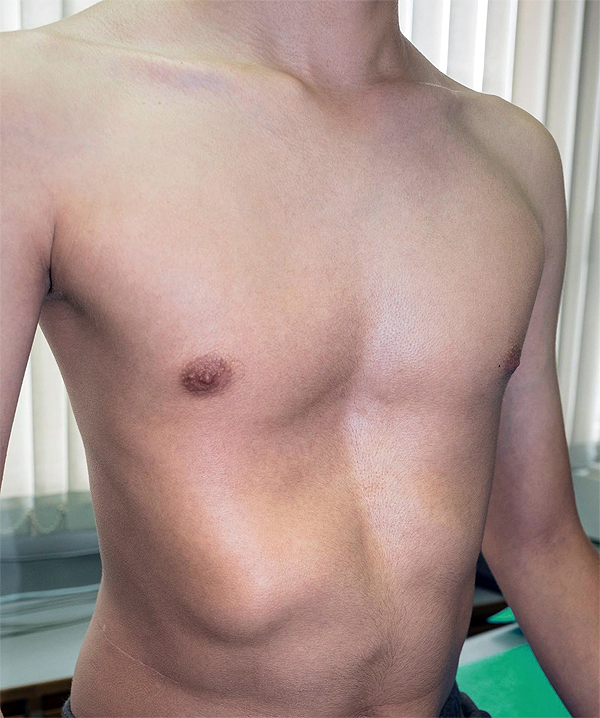
Pectus excavatum (PE) is an abnormal development of the rib cage, in which the breastbone caves in, causing the chest to “sink” inward. This developmental abnormality often presents at birth and can be mild or severe. Although the sunken chest wall deformity is most common in the middle of the chest, it may move to one side of the chest, usually the right. Pectus excavatum occurs more often in men than women, appearing in 1 per every 300 to 400 white male births.
Symptoms of Pectus Excavatum
Most patients do not have symptoms, though a minority of patients may have the following symptoms:
- Fatigue
- Shortness of breath/decreased exercise tolerance
- Chest pain
- Fast heart rate (tachycardia)
What causes Pectus Excavatum?
The causes of pectus excavatum are not well understood. It is thought that the deformity is due to excessive growth of the connective tissue that joins the ribs to the breastbone. This excessive growth may subsequently cause an inward defect of the sternum. If there is uncoordinated growth between the ribs and the chest, the ribs may grow faster than the expansion of the heart and lungs (which normally pushes the sternum outward), resulting in the sternum being pushed inward.
There are certain disorders associated with pectus exacavatum including:
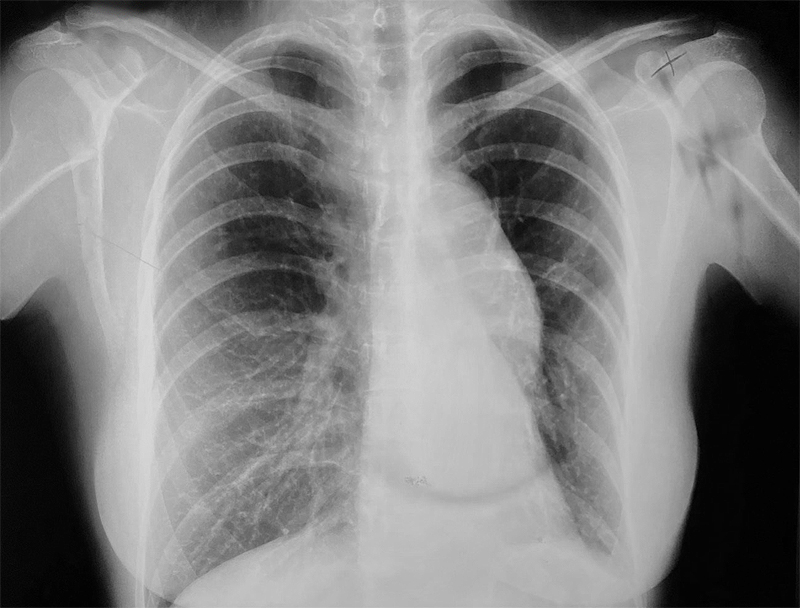
Marfan Syndrome
- A connective tissue disorder, which causes skeletal defects.
- Is typically recognized by long limbs and ‘spider-like’ fingers, chest abnormalities, and spine curvature.
Rickets
- Due to a lack of vitamin D or calcium and inadequate sunlight exposure, which destroys normal bone growth.
- This primarily occurs in children
Scoliosis
- This is the curvature of the spine
Tests and Diagnosis of Pectus Excavatum
- Complete Physical Exam
- Comprehensive Blood Tests, such as chromosome studies or enzyme assays
- Physical (stress) Tests
- Chest x-ray
- CT scan of the chest
- Electrocardiogram (EKG)
- Echocardiogram (picture of the heart)
Treatment of Pectus Excavatum
Since most patients with pectus excavatum do not have symptoms, treatment may not be needed or will be dependent upon the development of symptoms. If pectus excavatum is compromising to either the heart or lungs, your doctor may recommend surgery.
Surgery
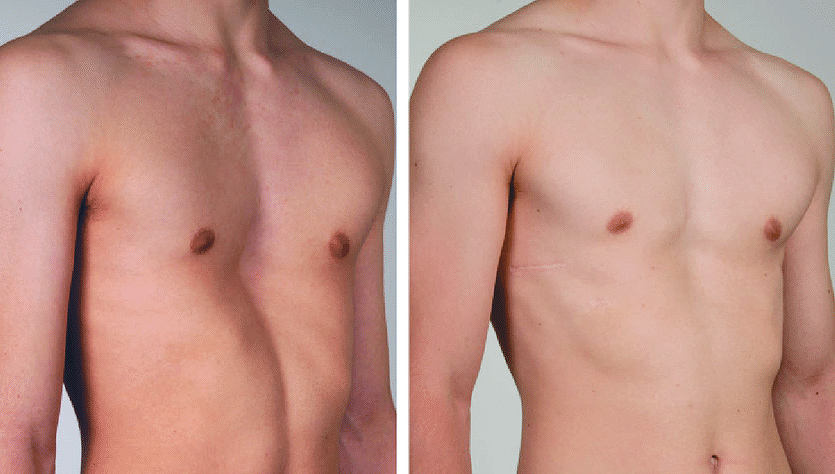
The primary goal of pectus excavatum repair surgery is to correct the chest deformity to improve a patient’s breathing, posture, and cardiac function. Removing a portion of the deformed cartilage and re-positioning the breastbone typically accomplish this. Repair of pectus excavatum is not recommended unless the patient has symptoms. Physical therapy in young patients may help in slowing the development of the chest wall deformity and may reverse some of the chest wall deformity.
Risks of Surgical Repair
- Pneumothorax (accumulation of air or gas in the pleural space)
- Bleeding
- Pleural effusion (fluid around the lungs)
- Infection
- Pectus excavatum recurrence
Rib Fractures
Fractured ribs (also known as cracked ribs), usually occur as a result of blunt chest wall trauma or lifestyle injuries that range from cycling to football. Fractured ribs may heal on their own without treatment. However, some patients have rib fractures in which bone fragments can damage major blood vessels, or structures like the lung, liver, kidneys, or spleen. In these cases, rib fractures usually require treatment.
Symptoms of a rib fracture may include pain with the following actions:
- Taking a deep breath
- Pressing on the injured area
- Bending or twisting your body
Risk Factors of Rib Fractures
- Osteoporosis – this disease decreases the density of your bones, making your rib more sensitive to fractures.
- Playing sports
- Having an area of cancer in your rib – cancer may weaken the bone, making your rib more sensitive to fractures.
Rib Fracture Diagnosis and Treatment
Diagnosis of rib fractures is achieved via X-Ray, CT scan, or MRI, which can also look at the organs and soft tissues around the ribs to detect damage to these areas. Most non-displaced fractured ribs heal without surgery in one to two months and are treated with non-surgical care that ranges from aggressive pain management to proper ventilation. For patients with displaced fractures, flail segments, or high narcotic requirements surgical treatment with rib plating may be required along with aggressive pain management and proper ventilation.
If you have questions regarding Chest Wall Conditions and Treatment, please call today. Click here to request an appointment.