If you have questions regarding LVRS Treatment, or Emphysema symptoms, please call today. Click here to request an appointment.
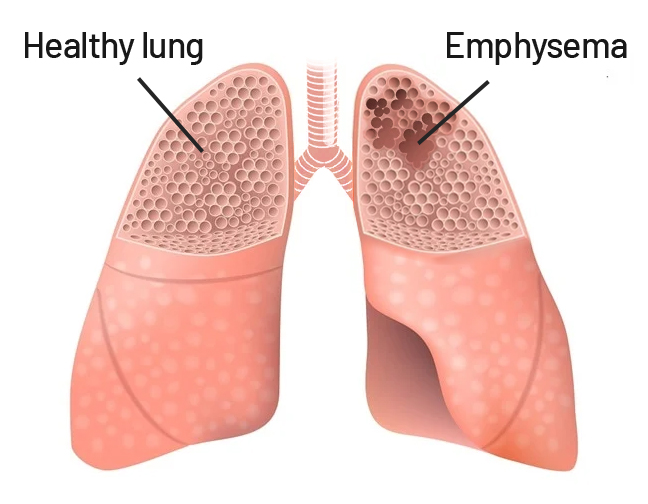
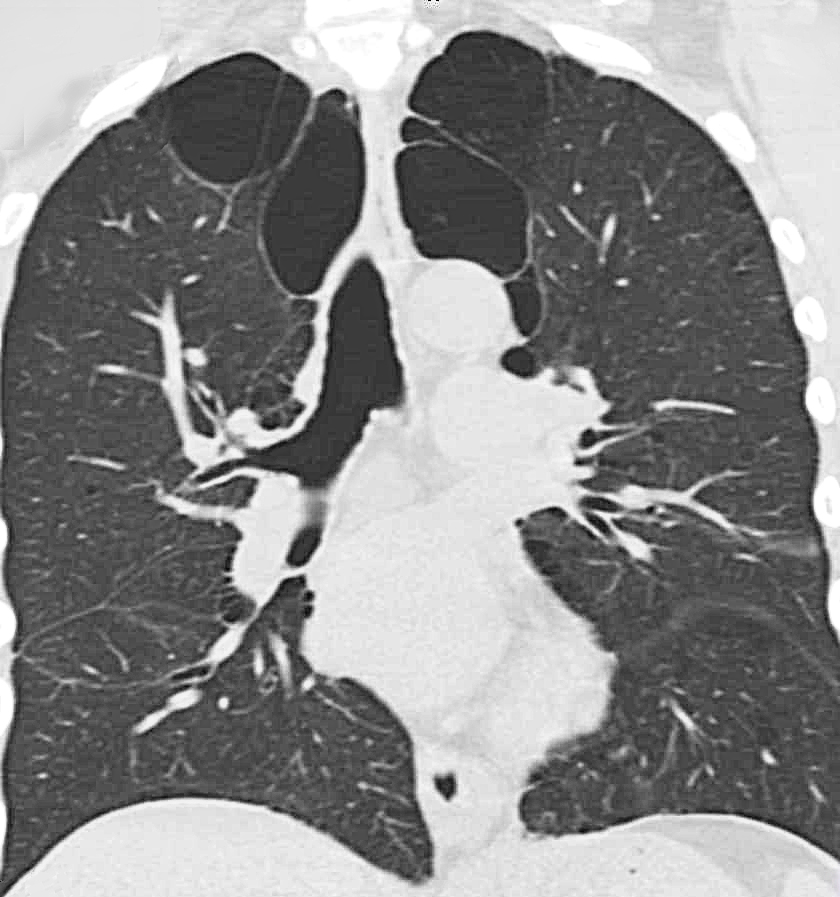
Lung Volume Reduction Surgery for Severe Emphysema
Lung Volume Reduction Surgery for Severe Emphysema
Schedule An Appointment
Saint John's: A Legacy of Care Excellence - Highly Awarded in 2024 and 2025 including COPD, Treatment of Pneumonia, Lung Cancer Surgery, and Pulmonology