Bladder cancer is more common than many realize, impacting 1 in 28 men and 1 in 91 women in the U.S. each year. Nearly 80,000 people receive this diagnosis annually, often with a history of smoking. At Providence Saint John’s Cancer Institute, patients aren’t treated in isolation—every case is reviewed by a team of experts across multiple specialties, ensuring care that is thoughtful, coordinated, and personalized.
What Is Bladder Cancer?
Most diagnosed with bladder cancer in the United States are over 70 years old. Men are 3-4 times more likely to present with bladder cancer than women.
There are two kinds of bladder tumors; benign and malignant. Benign tumors are not cancerous and do not invade the surrounding tissue. Once they are treated or removed, they usually do not grow back. Malignant tumors are cancerous growths. Although they can be removed successfully, they can also grow back.
Bladder cancer cells can invade nearby organs, such as the prostate in men or the uterus in women. They can also break away from the tumor and spread through blood vessels to other parts of the body, including the liver, lungs, bones, and lymph nodes. When this happens, cancer has metastasized (spreading that can lead to new tumors in other parts of the body).
What are the Signs and Symptoms of Bladder Cancer?
- Blood in urine (a rusty color)
- Feeling of an urgent need to urinate
- Having to urinate more often than you used to
- Feeling the need to urinate but with no results
- Needing to strain or bear down when you urinate
- Feeling pain when you urinate
These symptoms may also be caused by another health problem, such as an infection. If you are experiencing symptoms, make arrangements for treatment soon as possible.
What are the Risk Factors of Bladder Cancers?
Doctors have identified several risk factors for bladder cancer, which tend to be externally driven:
- Smoking is the biggest risk factor: The longer someone smokes, the greater the risk.
- Chemicals exposure such as in the workplace (working with dye, rubber, paint, metal, textiles, and leather industries may be at higher risk).
- People with cancer who have been treated with certain drugs, or who have had radiation treatment to the abdomen or pelvis, may be at higher risk.
- Caucasians are about twice as likely to develop bladder cancer as African Americans.
- Being over the age of 55
- Some studies have shown that a diet lacking sufficient amounts of fruits and vegetables can have a negative outcome for bladder cancer.

Careers with a higher risk of chemical exposure:
- Dry Cleaners
- Painters
- Autoworkers
- Truck drivers
- Paper manufacturers
- Metal workers
- Plumbers
- Hairdressers
- Tire and rubber workers
- Chemical and petroleum workers
How is Bladder Cancer Diagnosed?
To reach a diagnosis for bladder cancer, we take a thorough medical history and conduct a physical examination to be as accurate as possible. We will ask questions; make note of any symptoms you may have experienced and include any other pertinent information.
Dr. Jennifer Linehan discusses bladder cancer diagnosis and innovative methods.
The following tests may be used to diagnose bladder cancer or to find out if it has spread:
Urine tests:
A lab checks for blood, cancer cells, and other signs of disease.
Urine Cytology:
This method is used to identify cancer cells in the urine collected directly from the bladder.
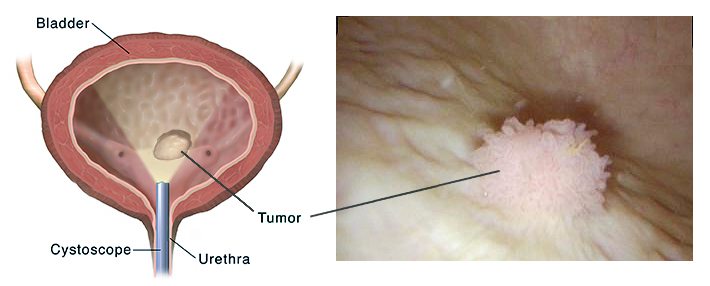
Biopsy:
A cystoscope is also used to remove tissue samples so that a pathologist can examine them for cancer cells. In most cases, a biopsy is the only sure way to tell whether cancer is 100% present.
If the biopsy finds cancer cells, the pathologist will determine the “grade” of the tumor. This may indicate how fast a tumor is likely to grow. Tumors with higher grades tend to grow faster and they are more likely to spread. Doctors use tumor grades along with other factors to suggest treatment options.
Cystoscopy:
A thin, lighted tube called a cystoscope is used to look directly into the bladder. Local anesthesia may be needed for this test because the cystoscope will be inserted into the bladder through the urethra.
Blue Light Cystoscopy
How blue light cystoscopy is transforming bladder cancer detection.
Blue light cystoscopy is an advanced imaging technique that uses a special dye absorbed by cancerous cells, causing them to glow bright pink under a blue‑light camera. This enhanced contrast helps doctors spot tumors that might be invisible under standard white light, including very small or flat lesions. The result is a more accurate, thorough evaluation of the bladder during diagnosis and treatment.
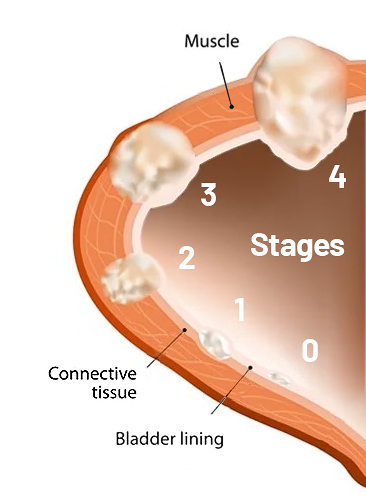
Bladder Cancer Staging
If you are diagnosed with bladder cancer, your doctor will determine the stage of the disease. Staging is a way of classifying cancer by how much of the disease is in the body and whether it has spread. This helps us plan the best way to treat the cancer. In the case of bladder cancer, staging is used to find out whether the tumor has invaded the muscle layer, nearby tissues, or more distant parts of the body.
Stage 0
At this stage, cancer is confined to the inner lining of the bladder. It has not invaded deeper layers or muscle tissue. Your doctor may call this carcinoma in situ.
Stage 1
Here, cancer has invaded the connective tissue beneath the bladder lining but has not reached the muscle layer.
Stage 2
Cancer has spread into the muscle of the bladder wall.
Stage 3
At this point, cancer has extended through the bladder muscle and into surrounding tissues or organs.
Stage 4
The tumor has invaded the wall of the pelvis or abdomen, but the cancer is not found in the lymph nodes. Or the cancer cells have spread to at least one lymph node or to parts of the body far from the bladder, such as the liver, lungs, or bones.
How is Bladder Cancer treated?
Treatment options for bladder cancer include surgery, intravesical therapy, chemotherapy, bladder sparing therapy, biological therapy, and radiation therapy. Our experts have performed thousands of laparoscopic and robotic-assisted surgeries, which help to reduce recovery time and side effects from treatment. Patients may receive more than one type of treatment depending on several factors, including the grade of the tumor, its location, and whether it has spread to other parts of the body. Before a treatment plan is determined, the following is taken into account:
Bladder Cancer Treatment Considerations
- Your age, overall health, and medical history
- The extent of the disease
- Your tolerance of specific medicines, procedures, or therapies
- Expectations for the course of the disease
- Your preferences for treatments
Treatment options are discussed so that you are as informed as possible when making treatment decisions.
Ways to Treat Bladder Cancer
At the Saint John’s Cancer Institute, we treat both early and later-stage bladder cancer. Primarily, we aim to preserve the bladder and spare the bladder from complete removal if possible. The treating physician performs the biopsy and performs surgery to remove the tumor from the bladder through the urethra. After recovery from this minor procedure, the patient returns to the clinic for a review of the pathology. This step allows for a more complete analysis of the tumor after it has been removed. If appropriate, weekly outpatient treatment begins. Common treatments include:
- Bladder Sparing Therapy (Trimodal Therapy)
- Surgery
- Radiation Therapy
- Chemotherapy
- Urinary Reconstruction and Diversion
- Intravesical Therapy
Bladder Sparing Therapy
Can you preserve the bladder having muscle-invasive bladder cancer?
Bladder‑sparing therapy is an approach for patients with muscle‑invasive bladder cancer that aims to treat the cancer without removing the bladder. For many years, the standard treatment was a cystectomy (bladder removal) often after chemotherapy. More recently, there has been significant progress in preserving the bladder, transforming treatment for muscle‑invasive cancer. This approach, called trimodal therapy, combines three components: chemotherapy (sometimes immunotherapy), surgery to remove as much of the tumor as possible, and targeted radiation.
Surgery
Surgery is an option for most people with bladder cancer. Surgical options vary based on individual factors, including cancer stage and overall health.
Transurethral resection (TUR):
This minimally invasive surgery is often used for early-stage bladder cancer. The doctor uses a cystoscope to treat early bladder cancer without any cutting or incision by inserting a scope through the urethra to remove cancerous tissue. TURBT is typically followed by intravesical therapy to prevent recurrence. This is a type of bladder sparing procedure.
Cystectomy
In more advanced stages, the surgeon may perform a partial or radical cystectomy. The surgeon may remove all or part of the bladder. Removing only part of the bladder is called a segmental cystectomy. The most common type of surgery involves removing the entire bladder, along with nearby lymph nodes and part of the urethra, which is called a radical cystectomy. After a radical cystectomy, reconstructive surgery is necessary. This may include creating a urinary diversion, such as a urostomy, which allows urine to exit the body through a stoma in the abdomen.
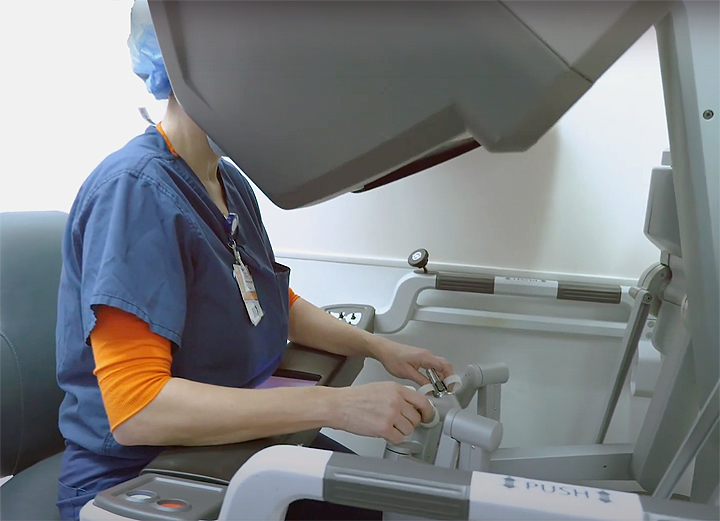
Robotic Bladder Cancer Surgery
This procedure is known as robotic-assisted cystectomy. The Saint John’s Cancer Institute specializes in robotic bladder surgery using the da Vinci Surgical System. In this procedure, we use a console to control miniature surgical instruments that are inserted into the body through tiny incisions. This minimally invasive surgery means less pain and a faster recovery.
Chemotherapy
Chemotherapy may be used to treat bladder cancer before or after surgery.
- Shrink the tumor before surgery
- Keep the cancer from recurring after surgery
- Prolong life when surgery is not an option
You may receive chemotherapy bladder tumor treatments in several ways:
Into the bladder:
After TUR for early bladder cancer, the doctor inserts a tube through the urethra to deliver medicine to the bladder. This treatment may be given once a week for six weeks.
Orally:
Some chemotherapy drugs are pills that may be given before or after surgery.
Intravenously:
For cancer that has invaded the muscle of the bladder or spread to other tissues, drugs are usually given intravenously via the arm.
Early Stage Immunotherapy Treatment
Patients with early bladder cancer may be able to receive a biological therapy (immunotherapy) called Bacillus Calmette-Guerin (BCG). It uses a weakened bacterium strain to stimulate the body’s natural defenses to attack the cancer. The BCG solution is inserted into the bladder through a catheter into the urethra. Once the solution comes in contact with the bladder tissue, this activates the body’s own immune system to eradicate the cancer.
Bladder Removal
When bladder cancer is extensive, requiring removal of the entire bladder, the surgeon creates another way for urine to be collected, stored, and released from the body. This is performed one of three ways.
Artificial Bladder
A surgeon uses tissues from the intestines to create what is known as a neobladder. The neobladder is attached to the urethra and allows the patient to urinate normally. At Saint John’s we are leaders in the field of this minimally invasive laparoscopic surgery which allows patients to return to normal physical activity much sooner.
Urinary diversion with a pouch inside the body
A surgeon uses intestinal tissue to create a reservoir called an Indiana Pouch with a path that leads out to the abdomen. The pouch collects urine inside the body. Several times a day, the patient uses a catheter (a soft tube) to connect to the path in the abdomen and empty urine in the Indiana pouch. Providence Saint John’s specializes in this procedure.
Urinary diversion with a bag outside the body
A surgeon uses intestinal tissue to create a path for urine to leave the body through an opening in the abdomen. This path is called a stoma. Its opening in the abdomen is covered by a bag that sits outside the body and catches the urine as it is released.
If you have questions regarding bladder cancer treatment, please call today. Click here to request an appointment.
Urology News and Health Information From Our Blog

Providence St. John’s Health Center
High Performing in Urology
Saint John’s Health Center is nationally ranked and in the top 10% for Urology
Learn more at Health.USNews.com.